Microsoft
Industry Solution Engineering (ISE)





The image was generated with Microsoft Create.
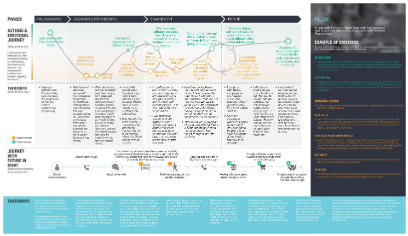
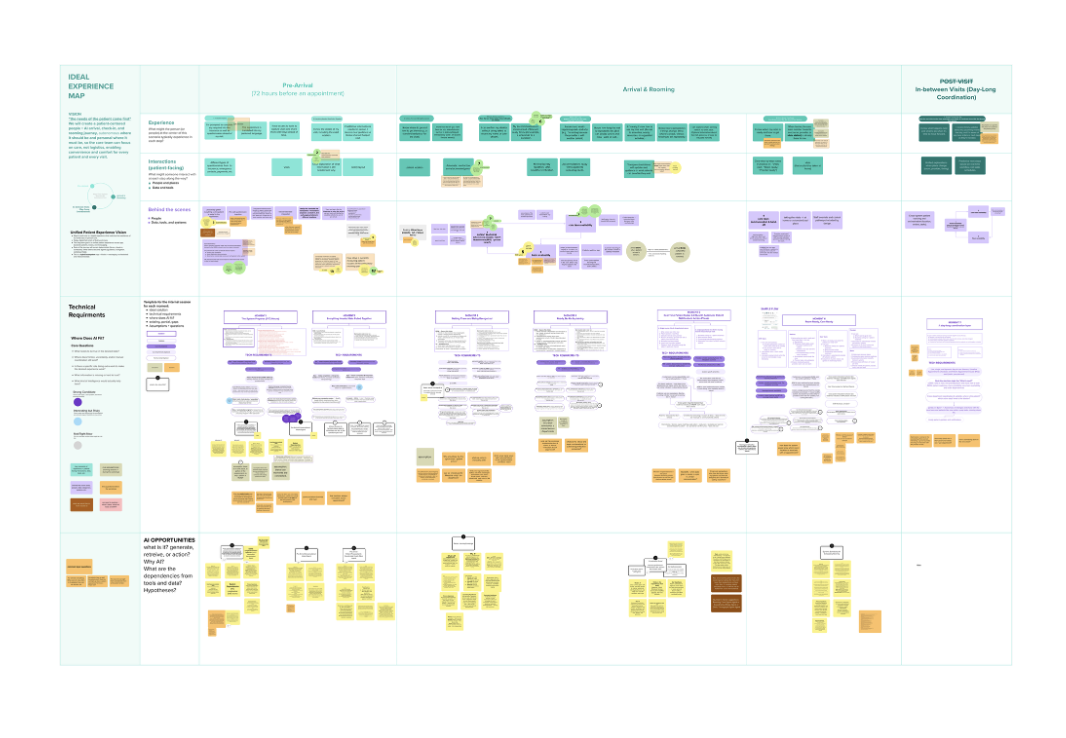
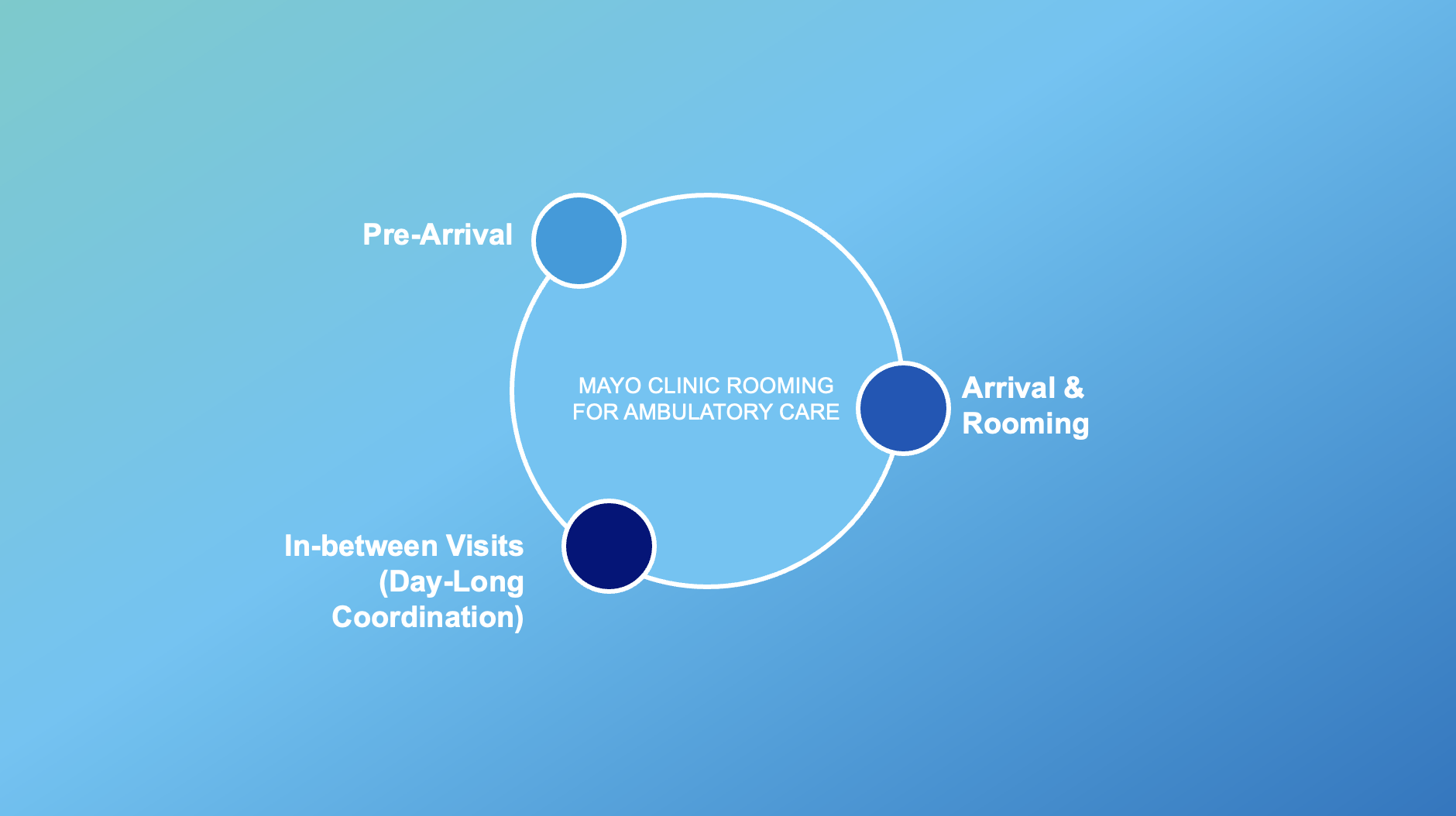
Reimagining ambulatory rooming and arrival through patient-centered, AI-enabled design
The problem
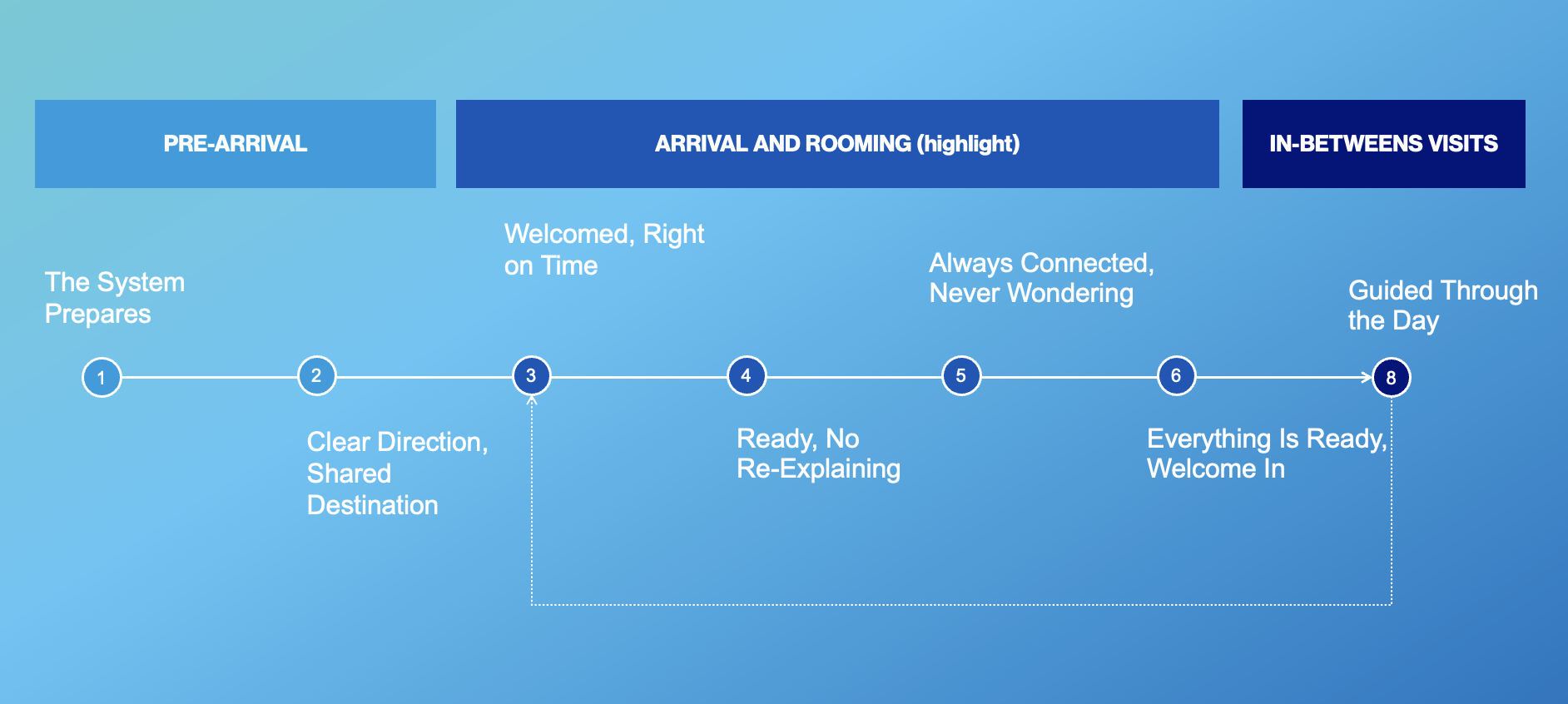
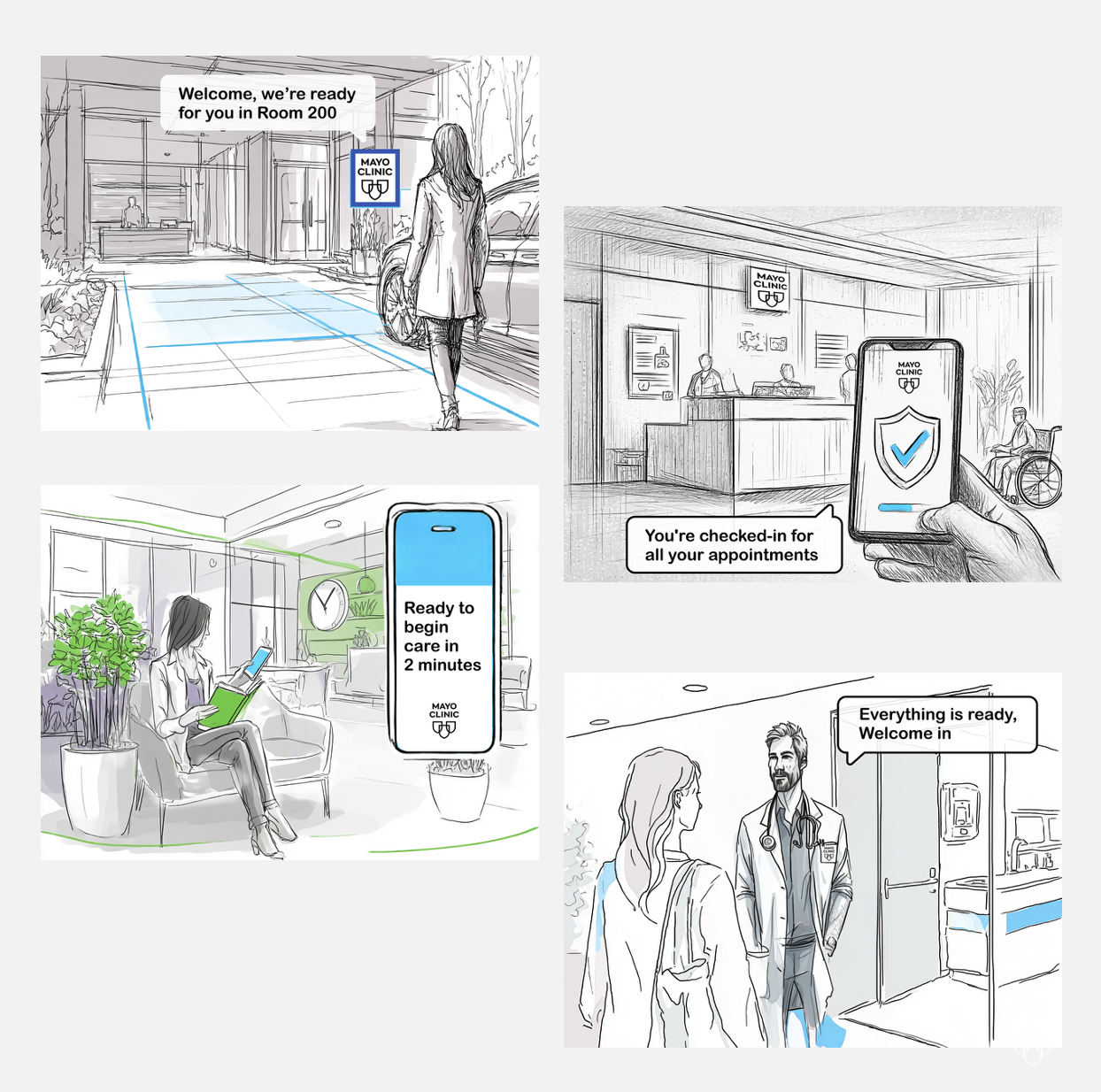
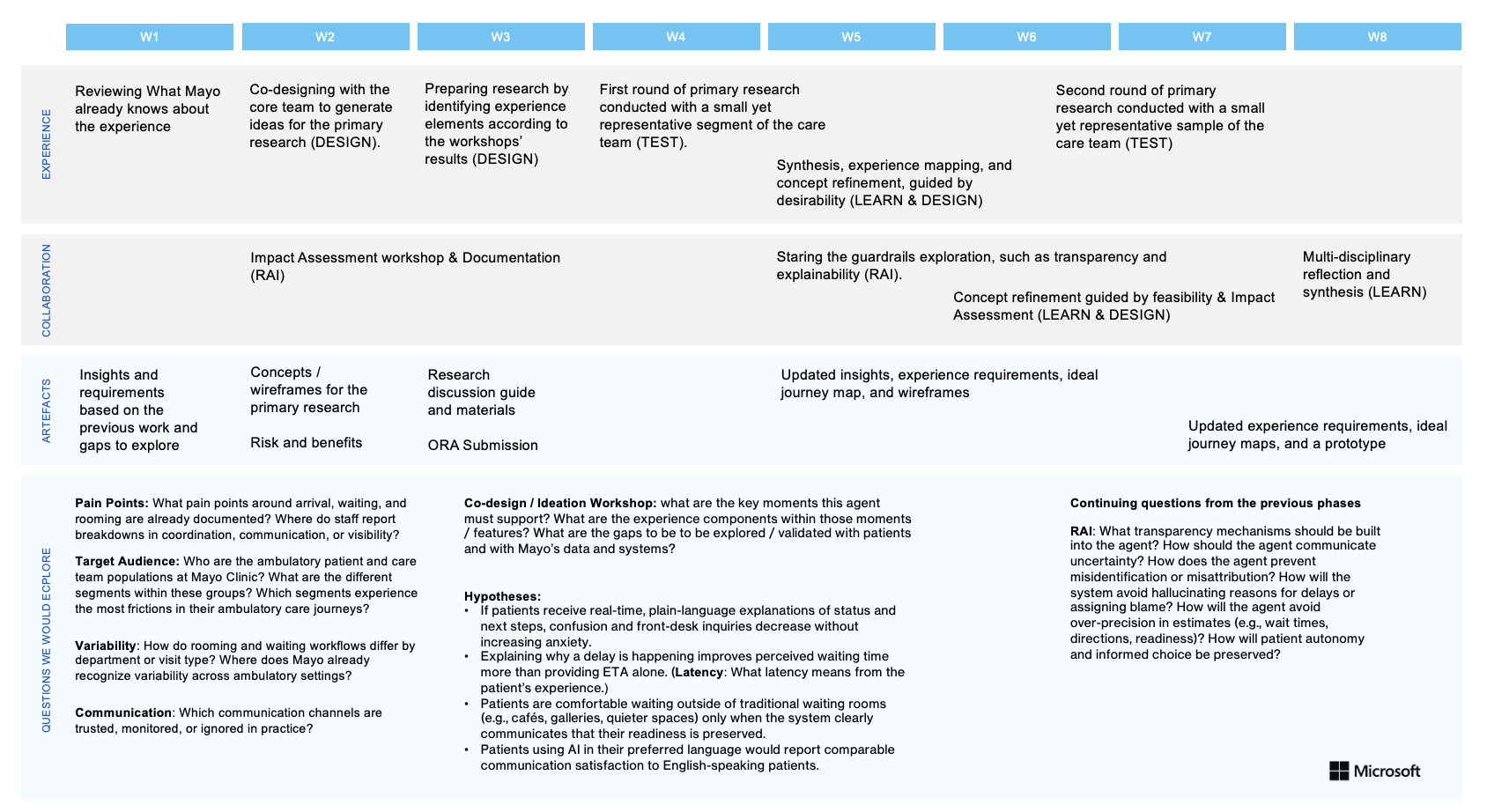
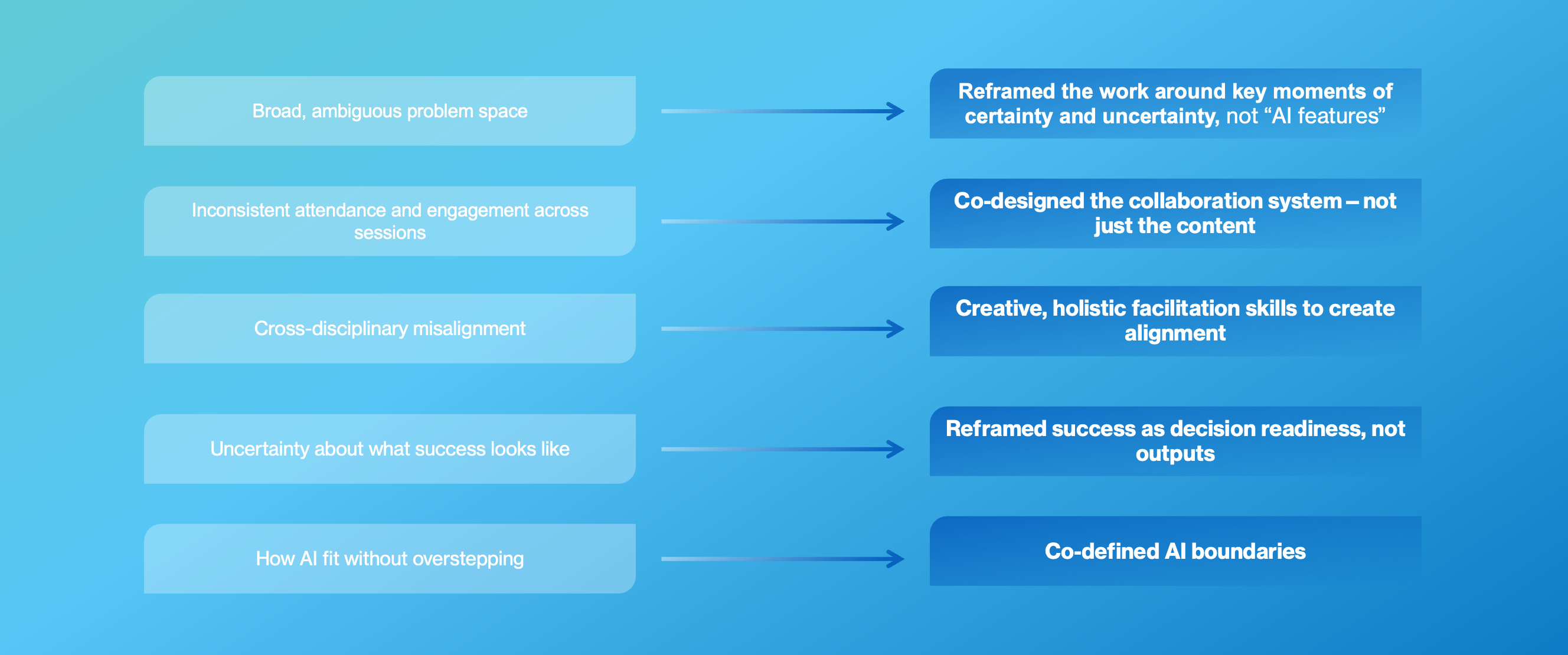
Ambulatory rooming workflows are high‑volume, time‑constrained, and cognitively demanding, placing significant documentation and coordination burden on care teams. Existing tools often obscure decision timing and workflow clarity, risking inefficiency while threatening clinician judgment, patient safety, and trust in outpatient settings.
Systems design
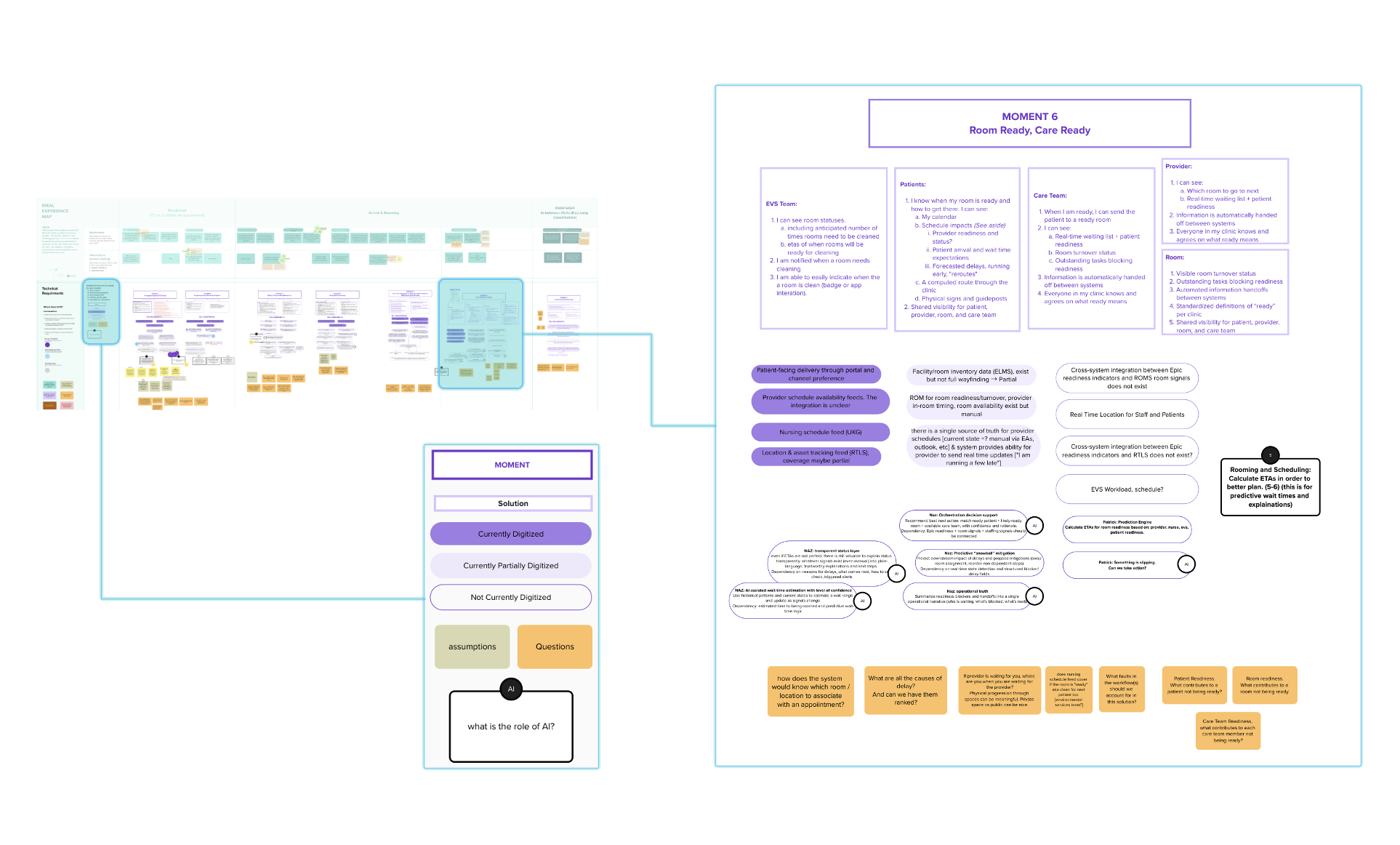
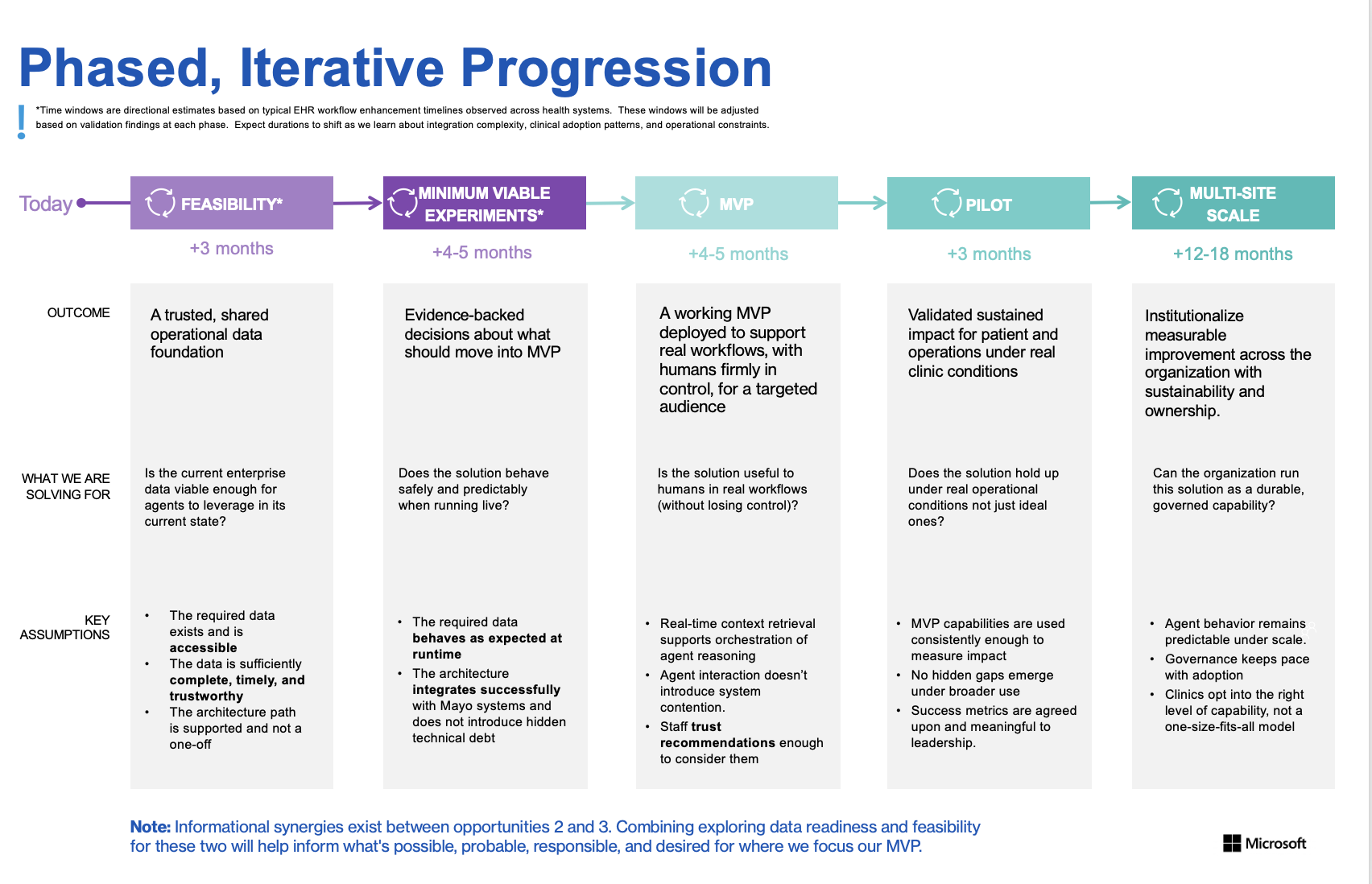
I led a multidisciplinary, participatory design engagement, working closely with clinicians, operational leaders, data science, and product partners to identify and shape AI‑enabled opportunities within ambulatory rooming workflows. Through field visits, journey mapping, and co‑design workshops, we synthesized clinical realities with technical constraints to define high‑value intervention points. The resulting system vision emphasized augmenting, not automating, clinical work, clarifying decision moments, reducing cognitive and documentation burden, and integrating AI responsibly into existing workflows. Insights were translated into a phased, responsible roadmap, balancing desirability, feasibility, viability, and safety.
Impact
The work aligned clinical, operational, and technical stakeholders around a shared vision for AI‑enabled ambulatory care and informed leadership investment decisions. The roadmap established a foundation for piloting and scaling responsible AI solutions across outpatient settings, with clear principles for trust, workflow fit, and clinical autonomy.

The image was generated with Microsoft Create.
Designing an assistive AI in a variable, regulated care management workflow without breaking human accountability
The problem
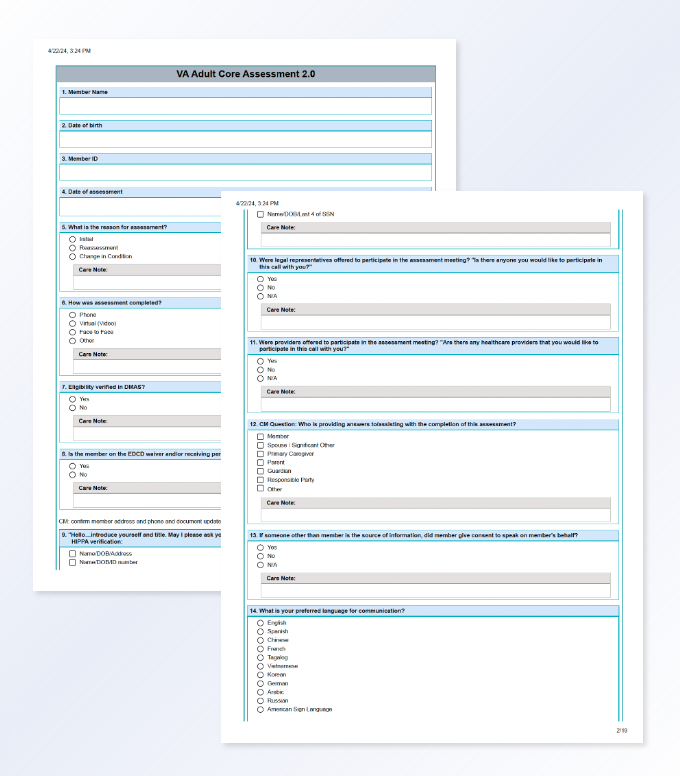
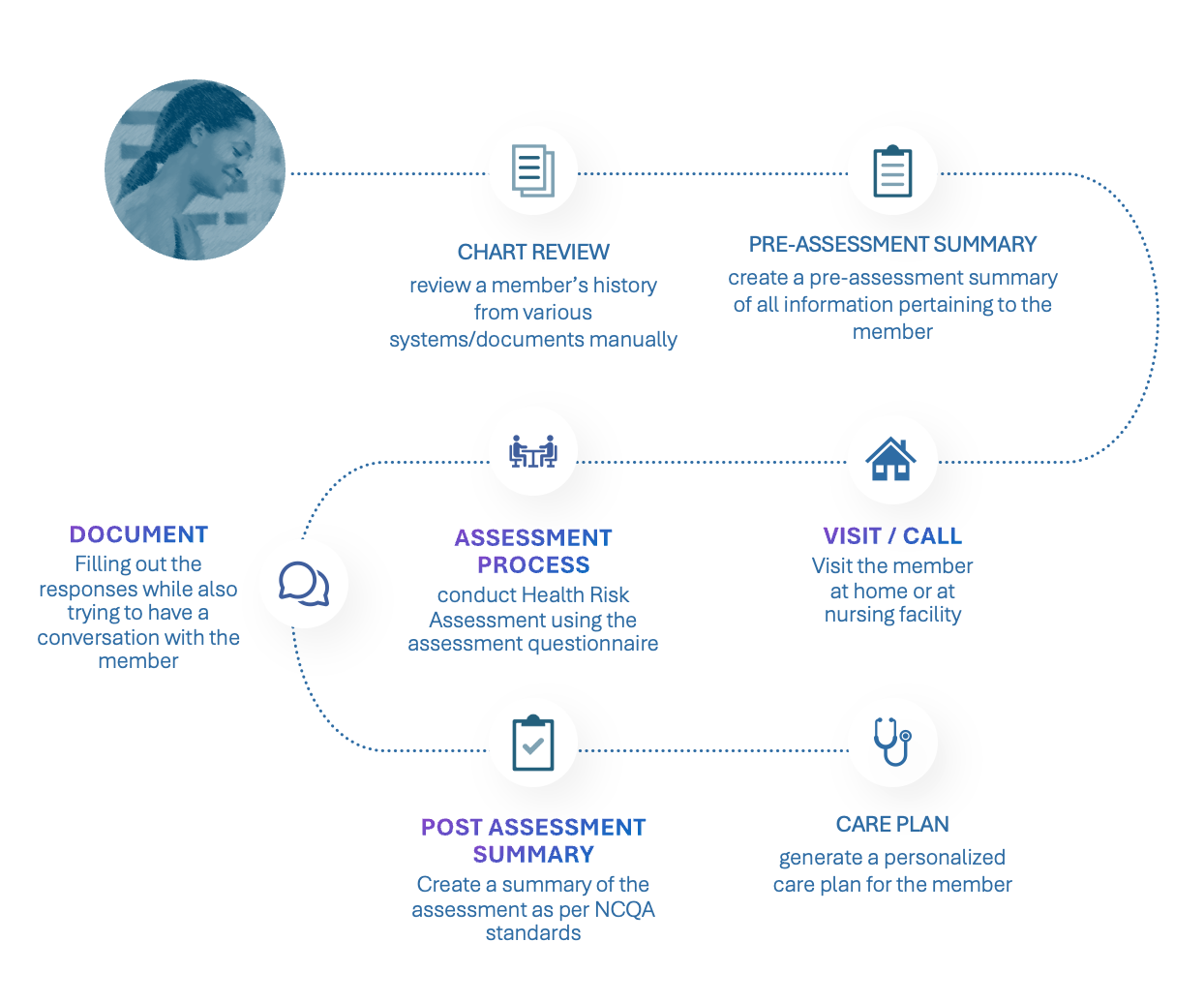
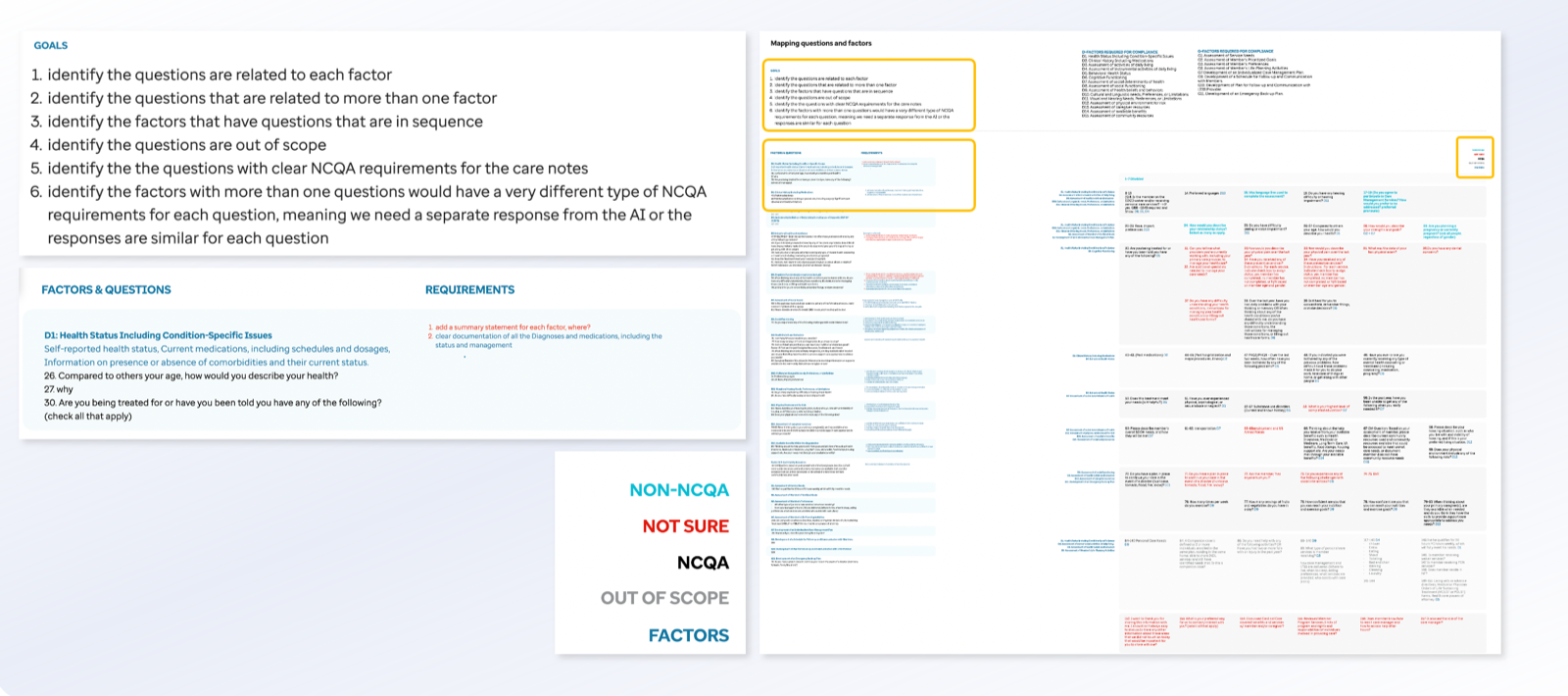
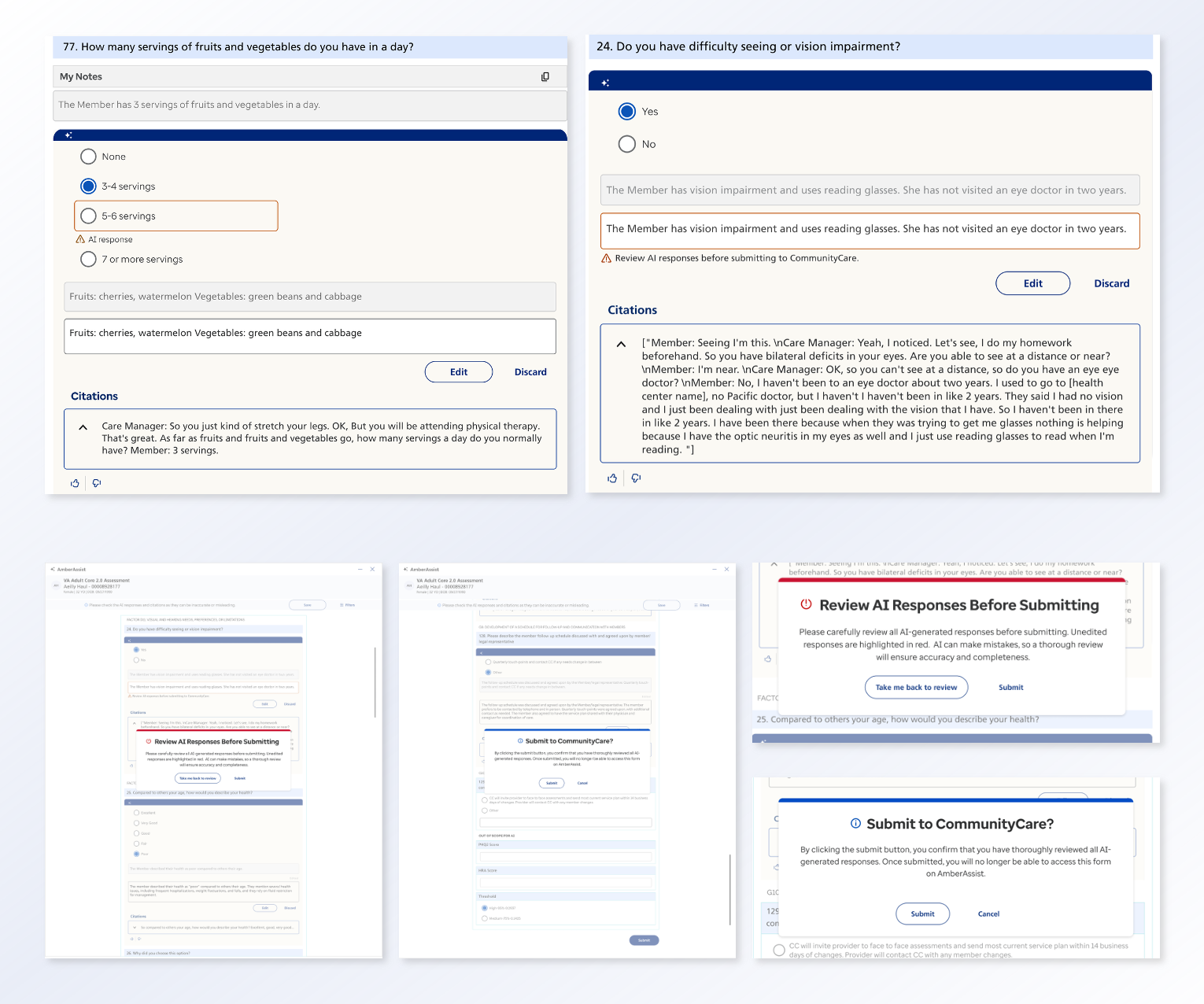
Care managers supporting Medicaid populations must synthesize fragmented member information while completing lengthy health risk assessments under regulatory constraints. Manual documentation processes are time‑consuming and prone to omission, increasing cognitive burden and reducing time available for meaningful member interaction.
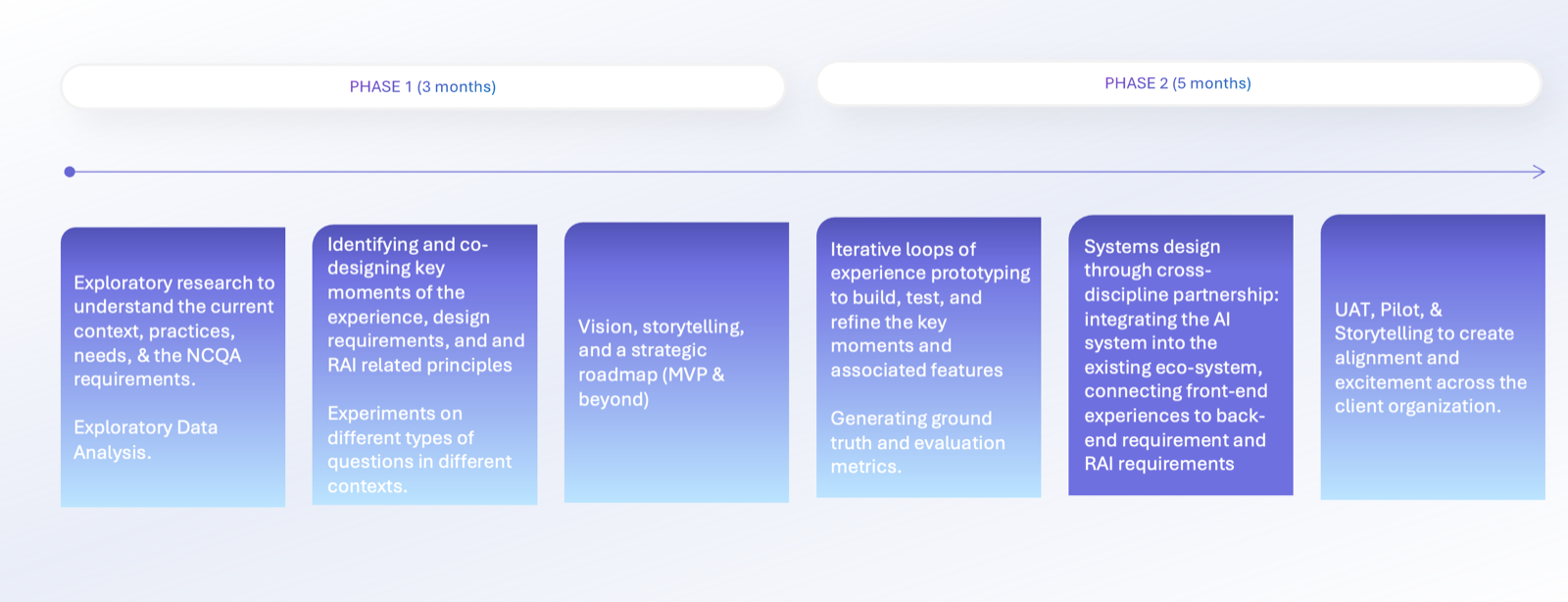
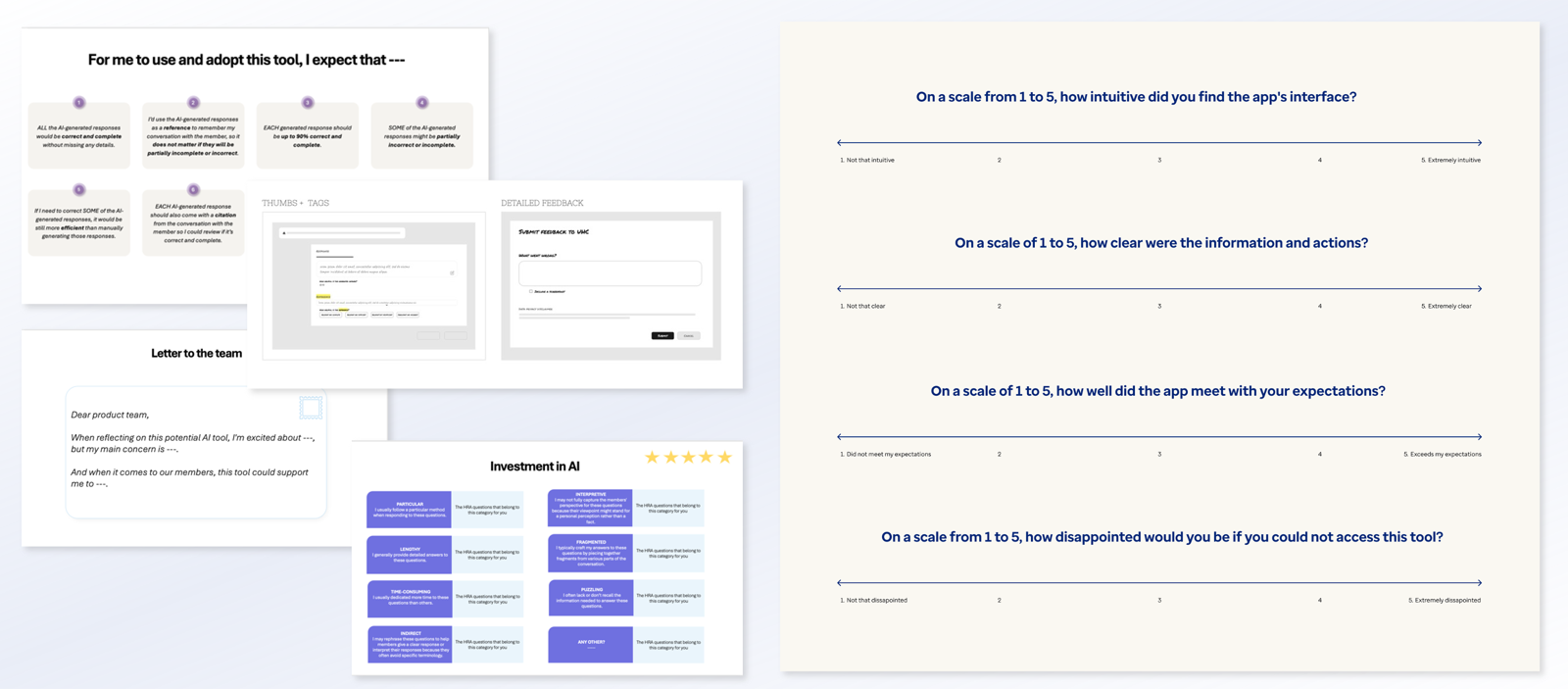
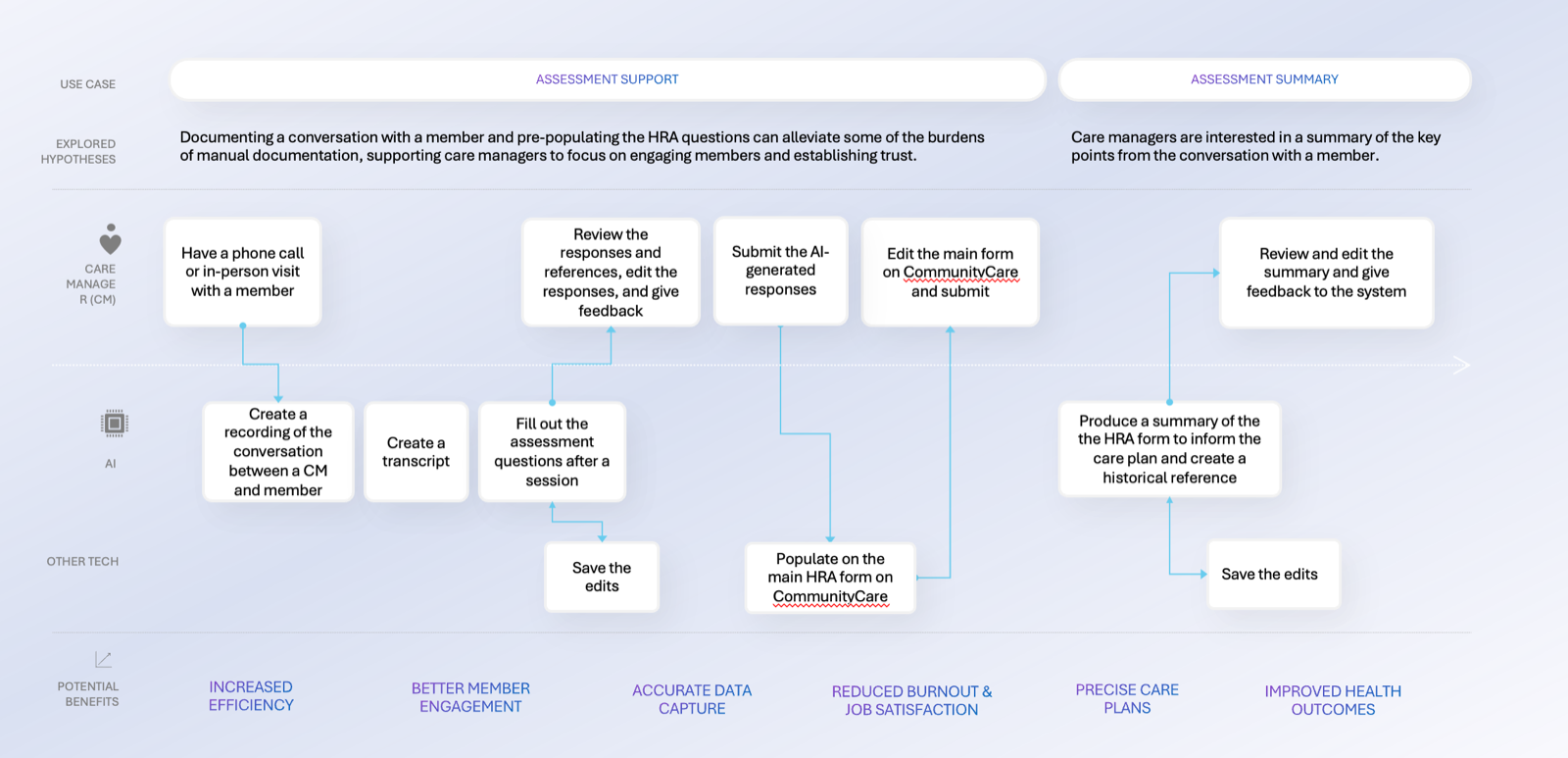
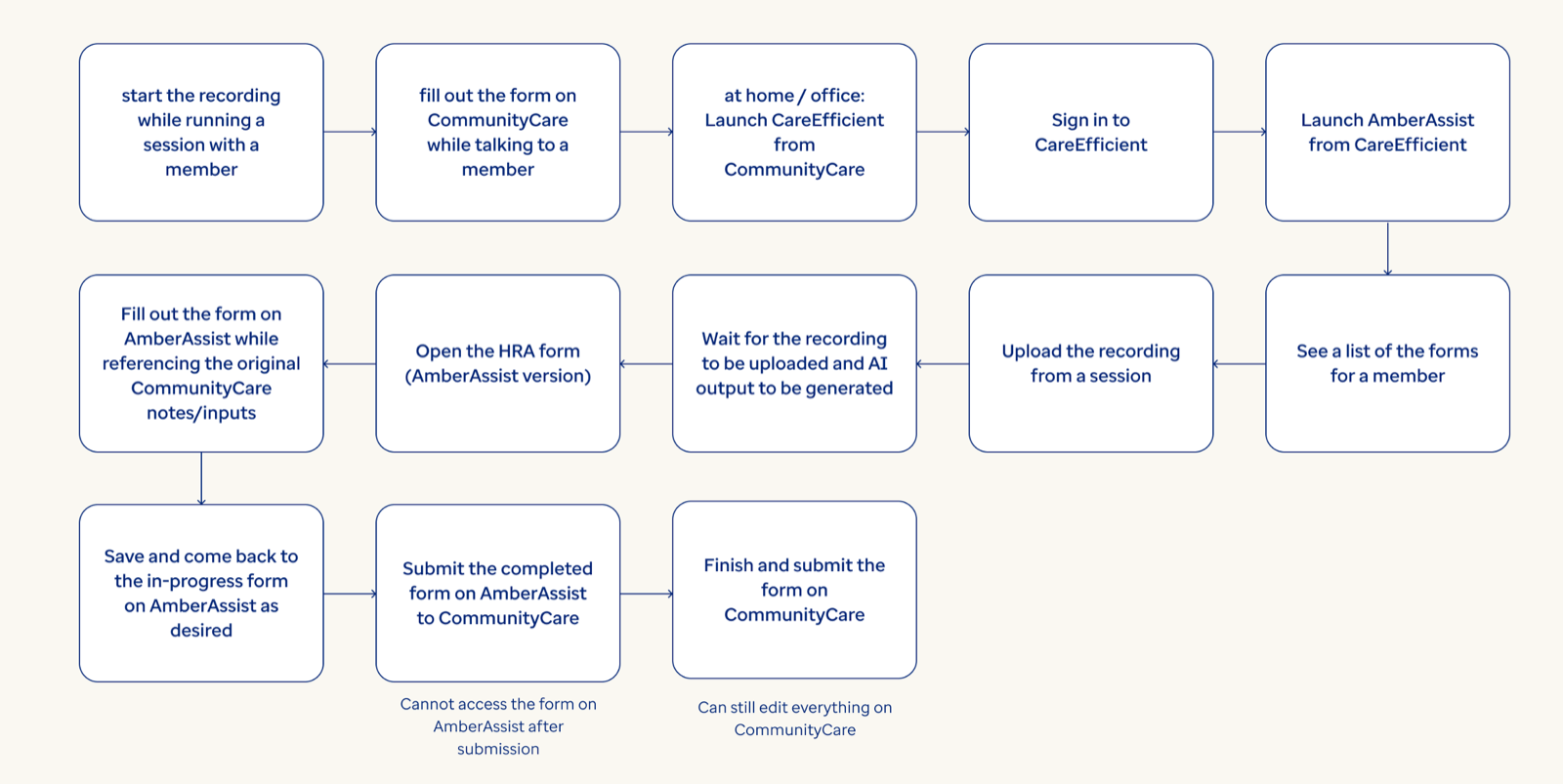
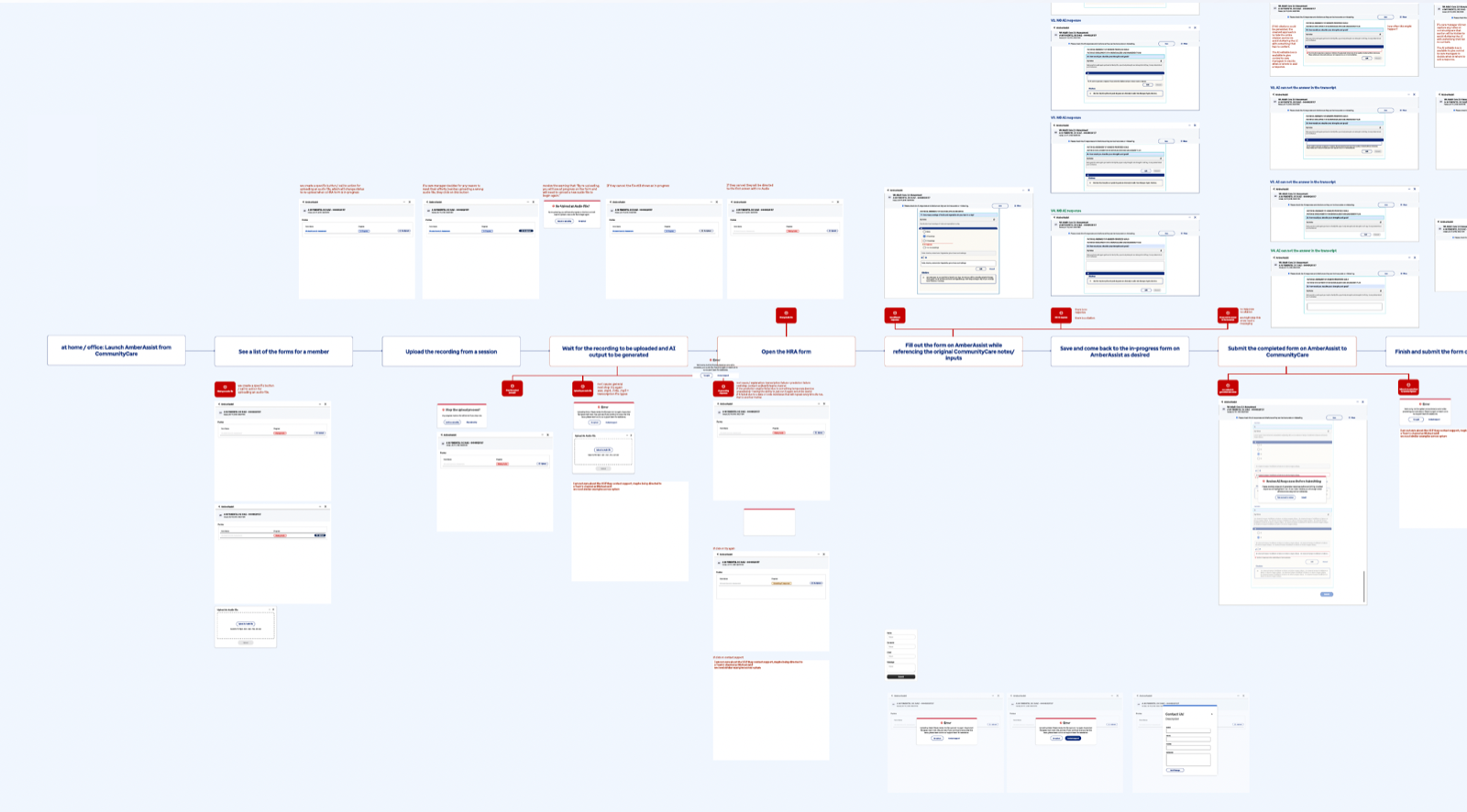
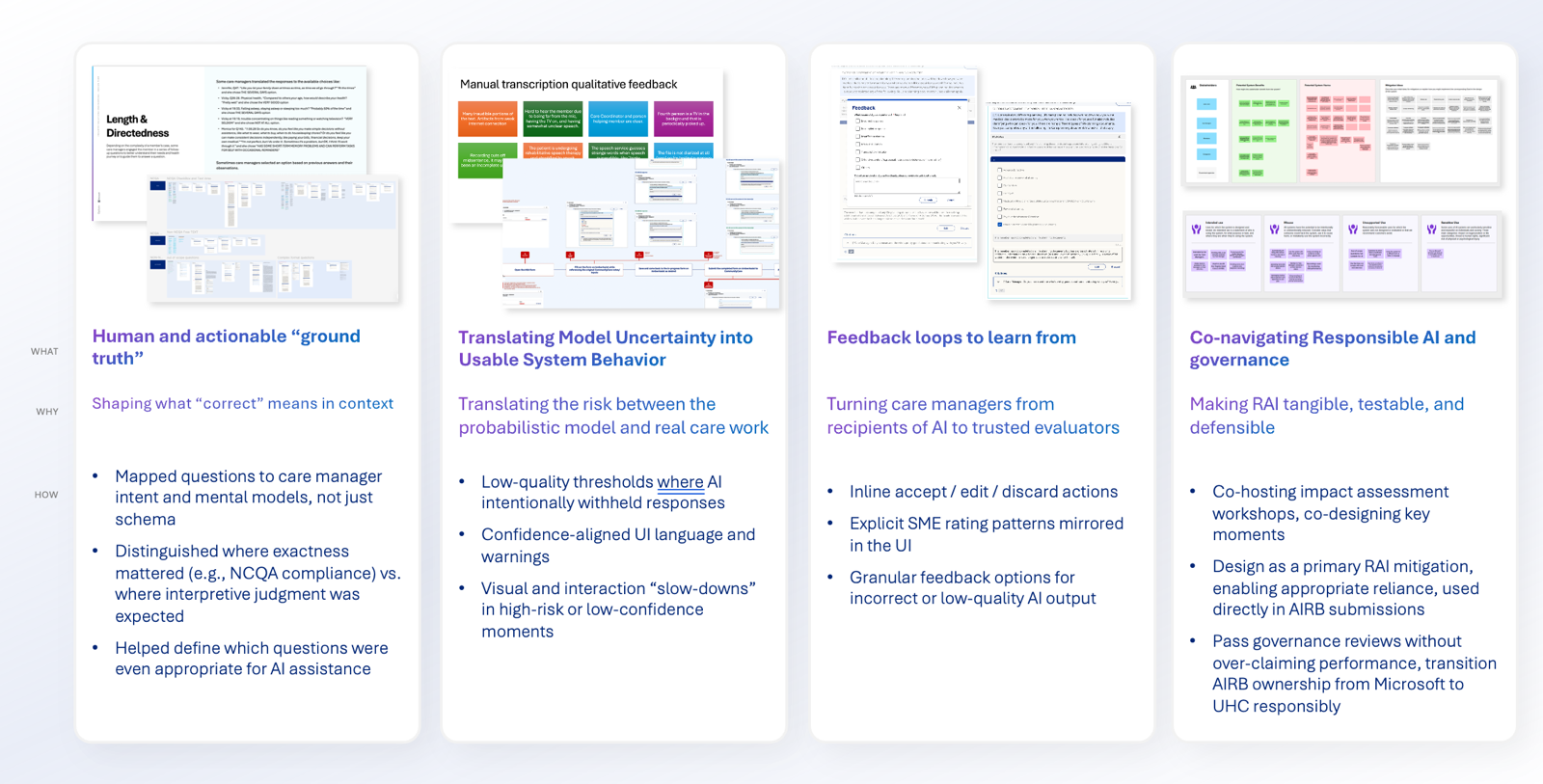
Systems design
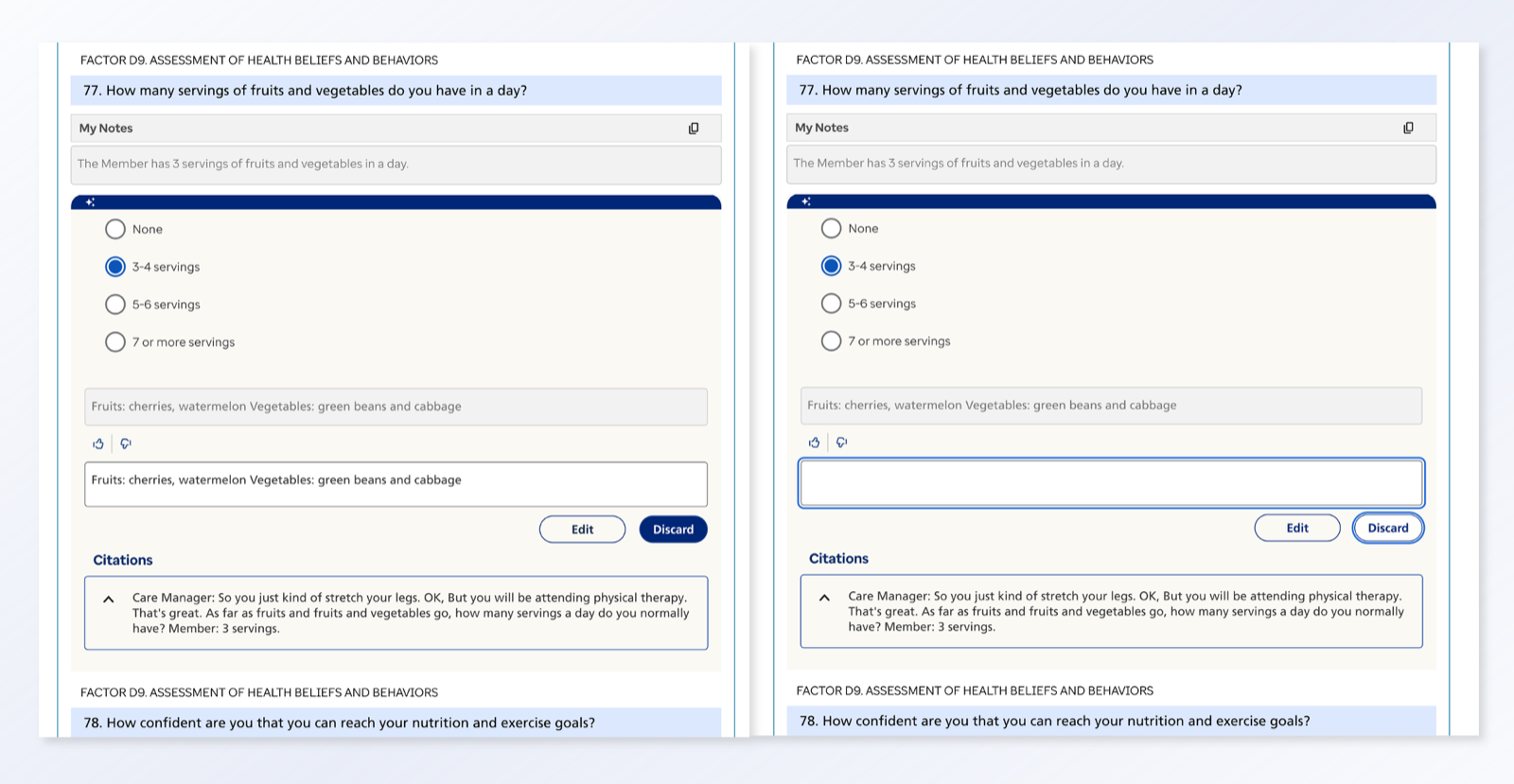
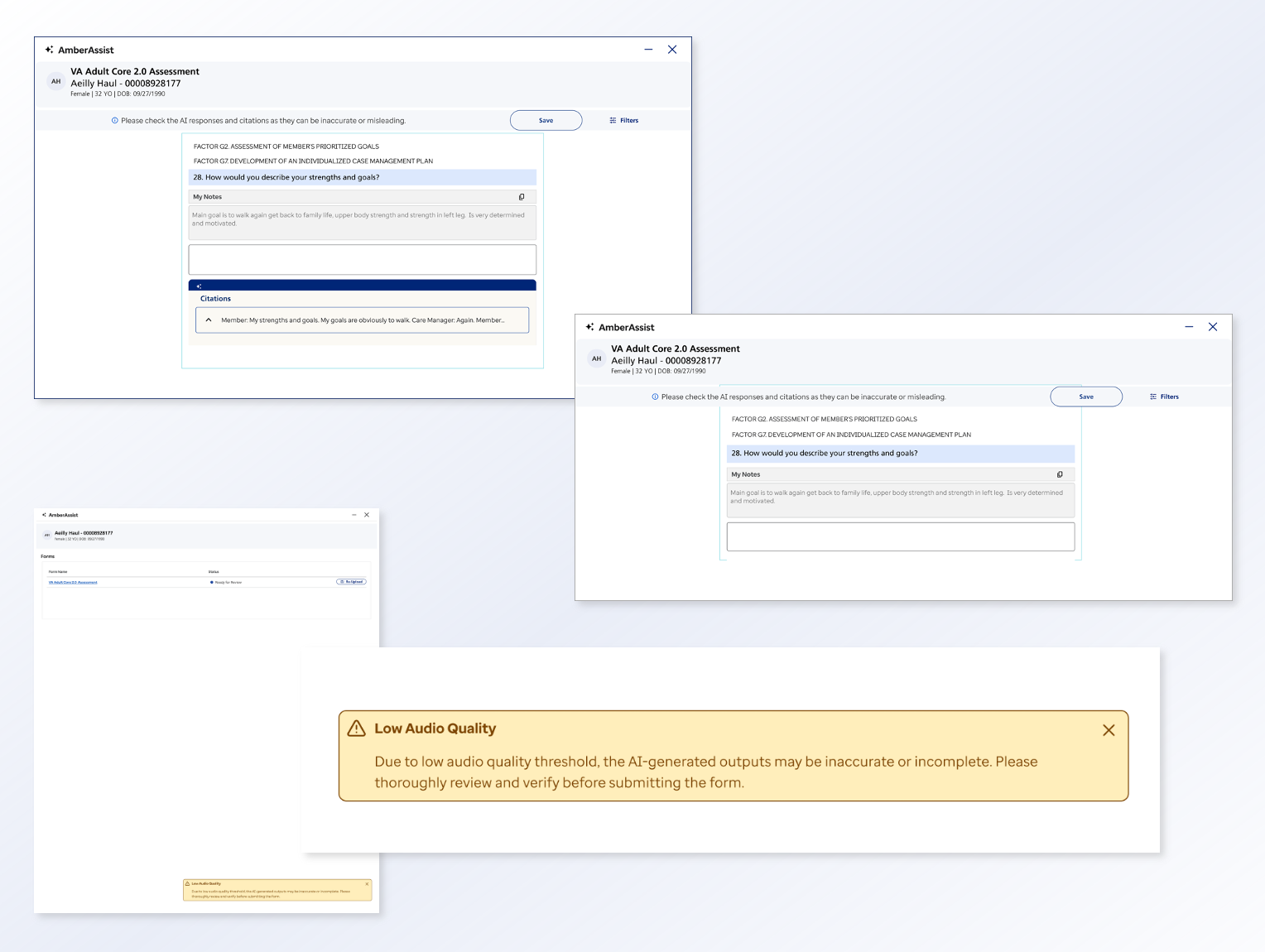
I led a design effort in close collaboration with care managers, data scientists, product, and engineering to design an MVP to support assessment completion. The system consolidates historical member data and pre‑populates assessment responses for human review, enabling care managers to edit, accept, or discard AI‑generated content with appropriate transparency. Grounded in RAI principles, design decisions framed AI as decision support rather than decision replacement, protecting areas requiring human judgment. Front‑end interactions were intentionally connected to transcription quality, data readiness, and compliance expectations to support appropriate reliance and informed oversight.
Impact
Design choices encouraged vigilance and accountability while improving workflow efficiency. Following the MVP, experience patterns are now being replicated across additional assessment forms and expanded to other state programs, enabling scalable, human‑AI collaboration in Medicaid care management nationwide.

Source: Adobe Stock
Augmenting clinician risk assessment through AI‑enabled decision support
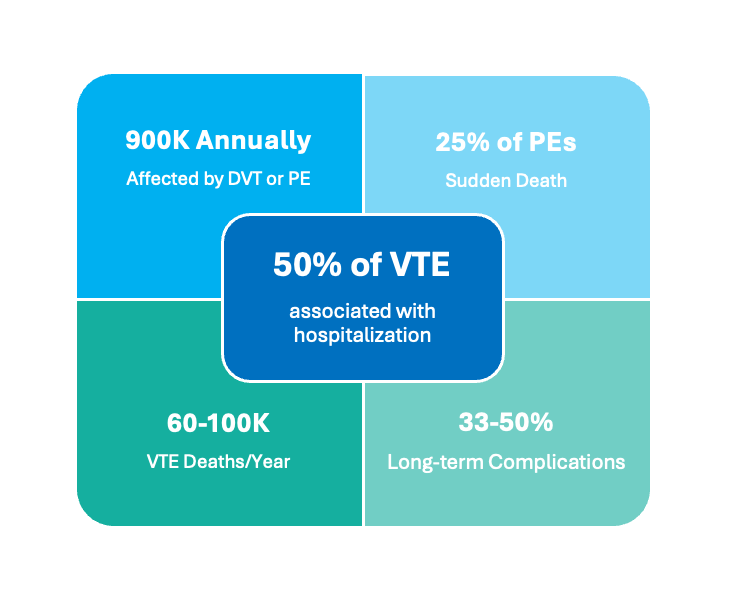
The problem
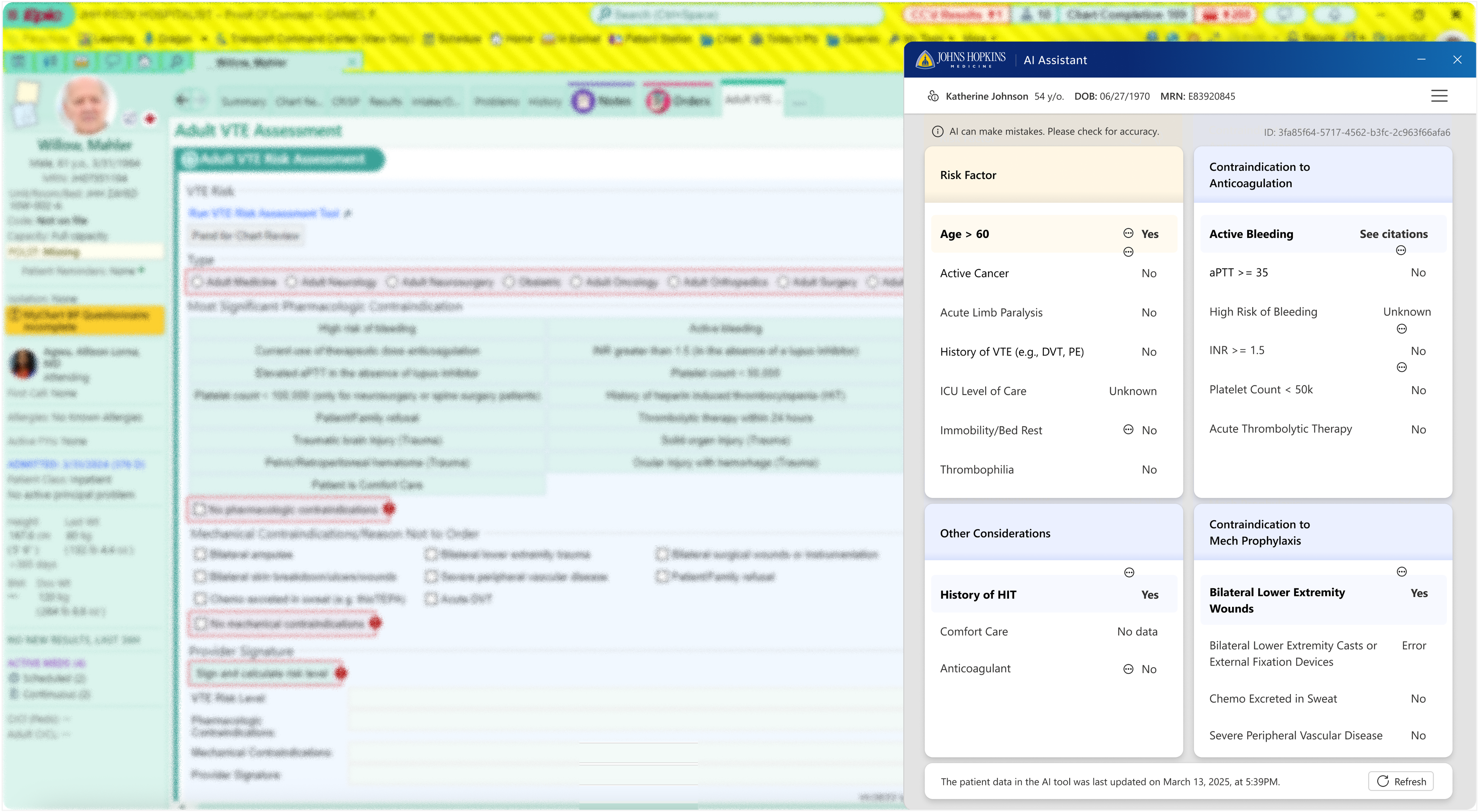
Clinicians must assess blood clots risk using fragmented, unstructured patient data under severe time pressure. Existing tools added friction and were often bypassed, forcing physicians to rely on memory and heuristics, introducing variability, inaccuracy, and risks, especially in complex cases.
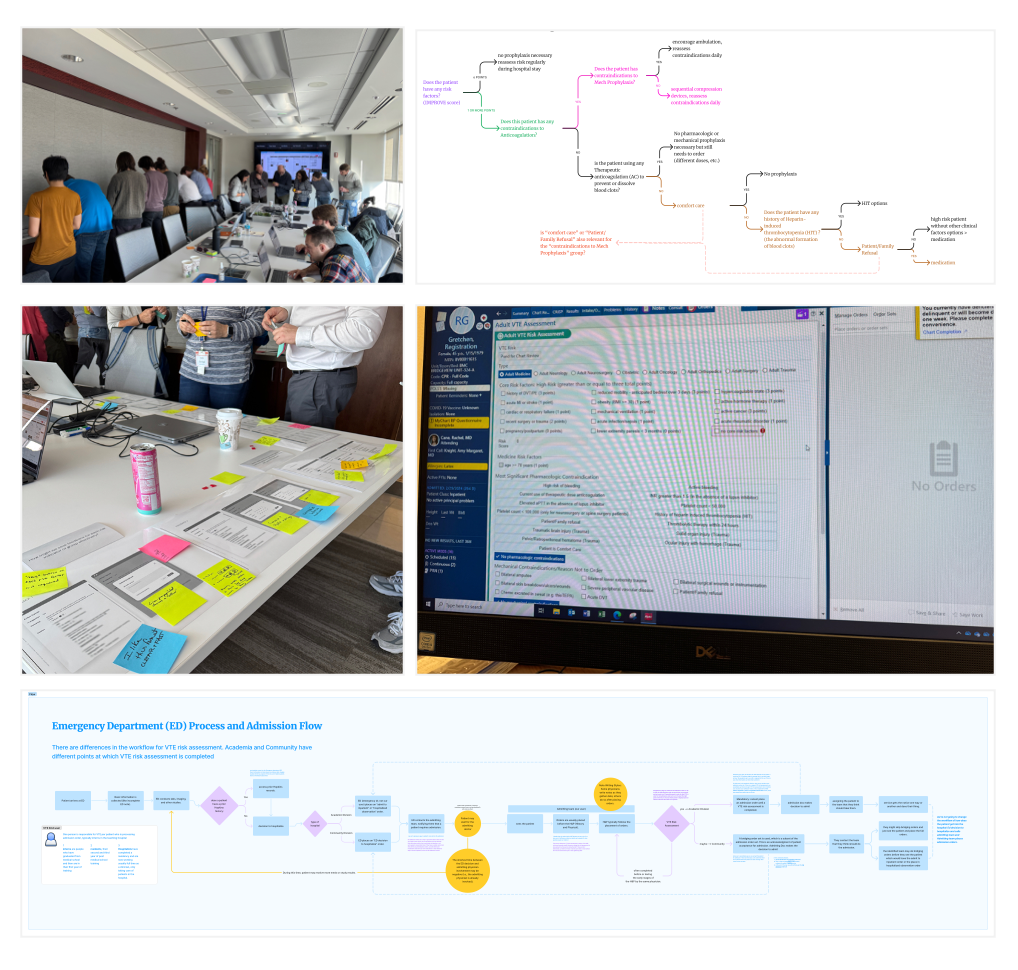
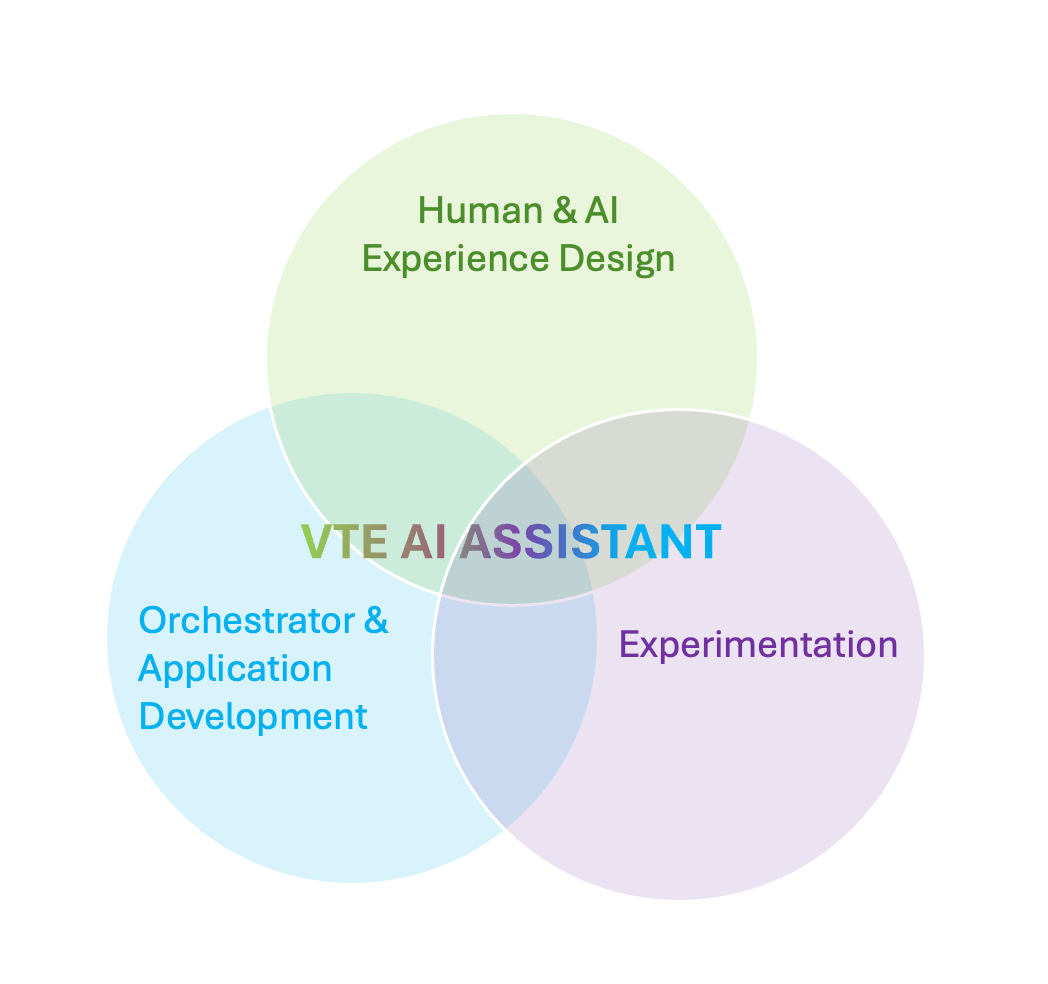
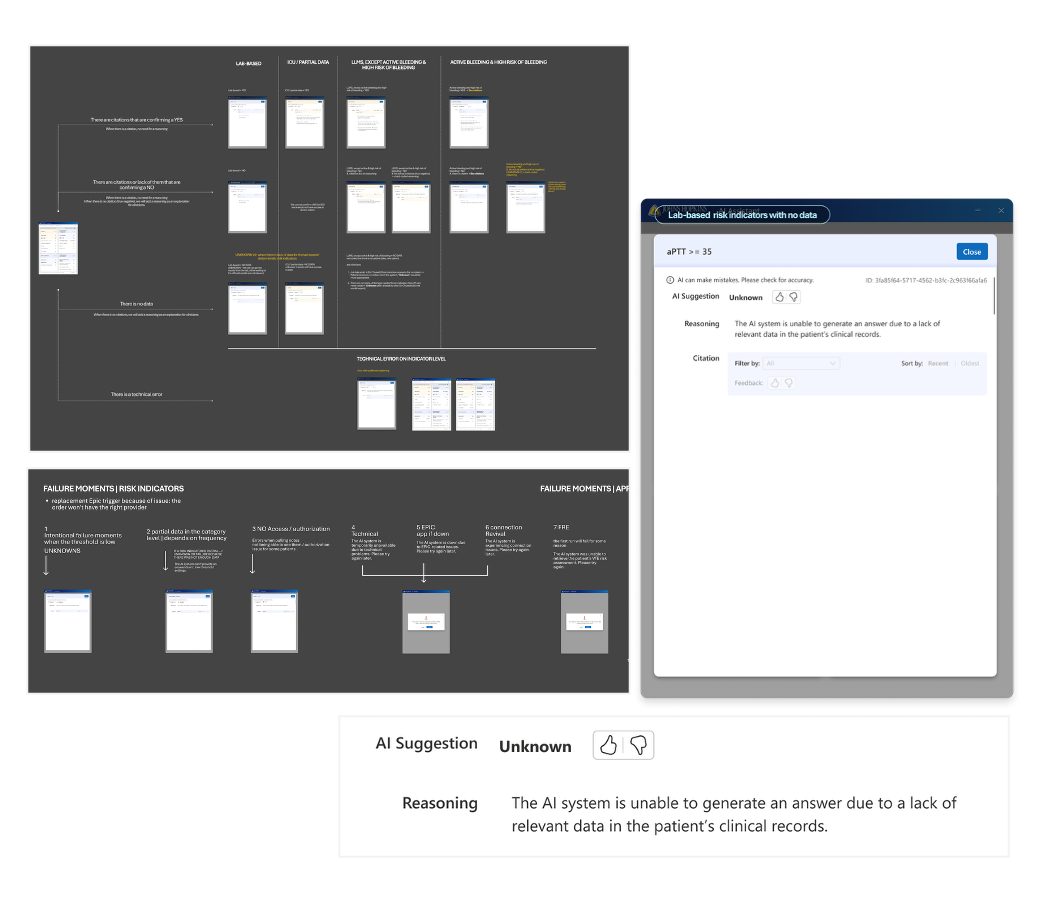
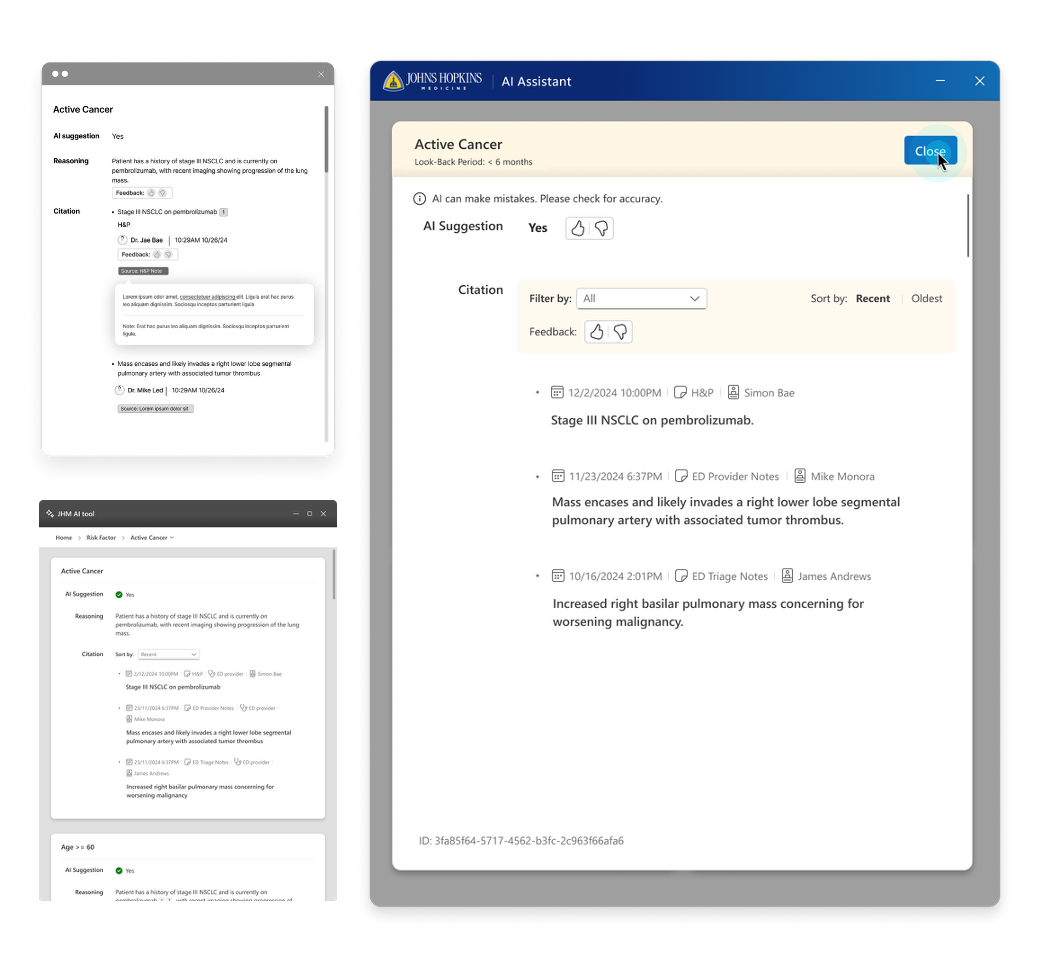
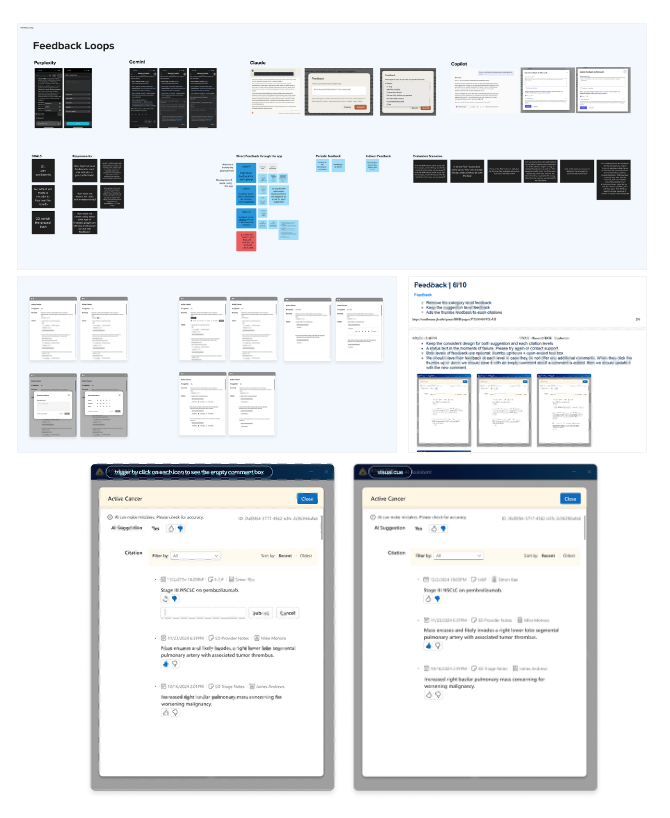
Systems design
Through a multidisciplinary, participatory design process, I partnered closely with physicians, data science, product, and engineering to design and deliver an AI‑assisted MVP that augments, not automates, clinical judgment. The system synthesizes and prioritizes patient‑specific risk signals, surfacing the most relevant context at the moment of decision‑making through reasonings and citations. Design choices intentionally preserved clinician autonomy while supporting guideline‑concordant care, ensuring the tool fit seamlessly into existing workflows and earned trust in high‑stakes clinical settings.
Impact
The MVP demonstrated value in reducing cognitive burden and improving clinician confidence, leading to scaling across the health system. The work established a repeatable model for responsible, human‑centered AI adoption in inpatient care.

Source: Adobe Stock
Accelerating learning and production for novice 3D artists through generative AI
The problem
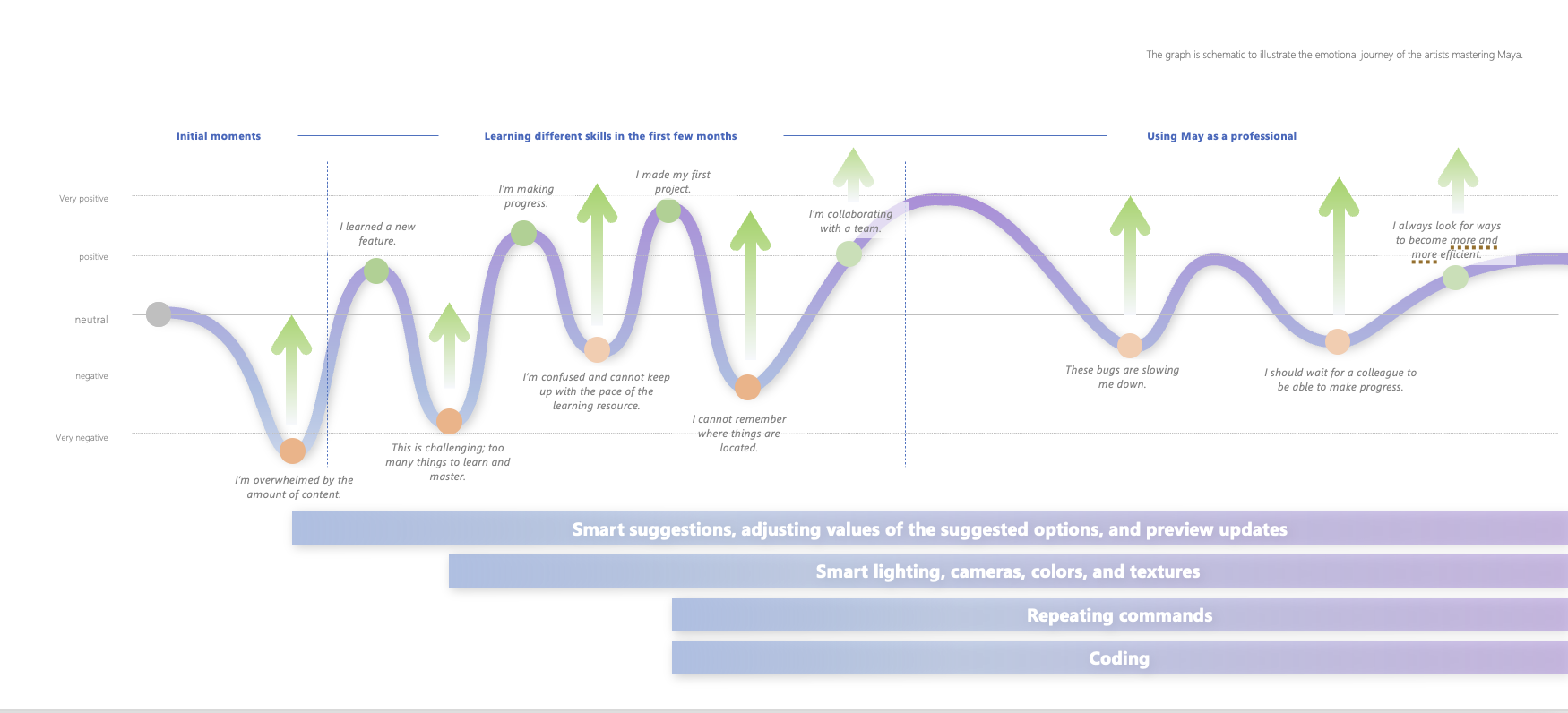
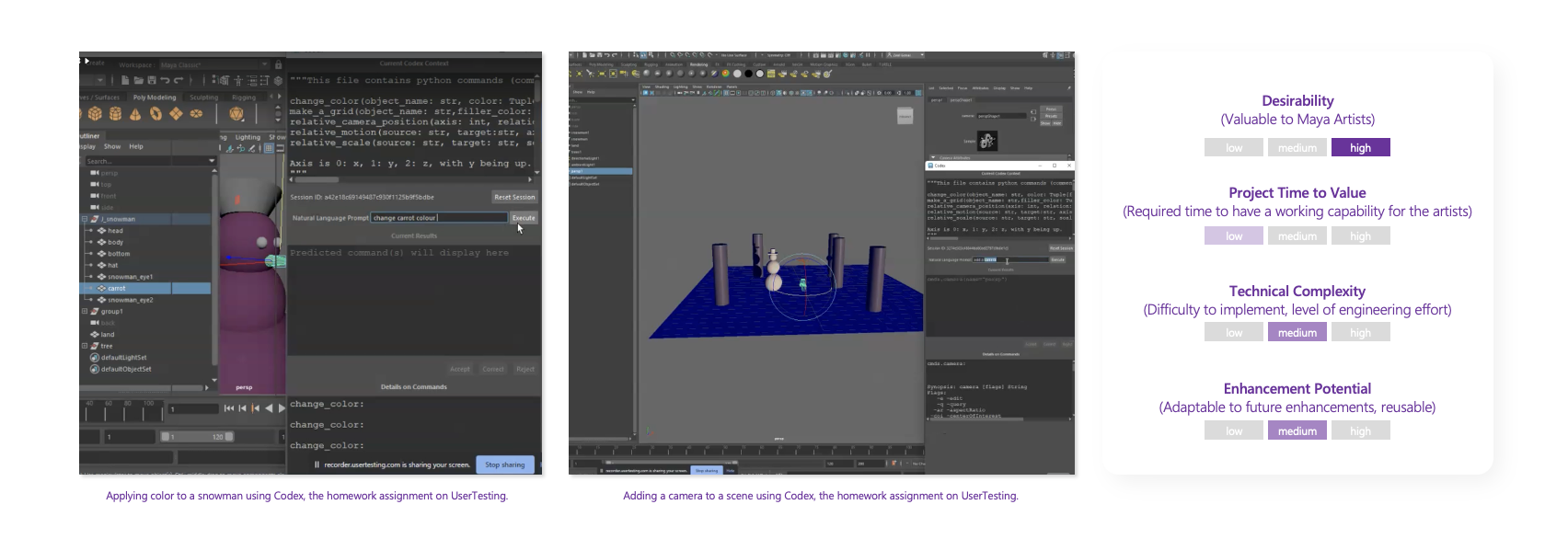
Novice and transitioning 3D artists often experience steep learning curves when using professional creative tools such as Autodesk Maya. New users frequently interrupt their workflows to consult external tutorials or forums, slowing skill development and production progress. At the same time, early research revealed resistance to AI automation, participants expressed concern that handing over creative control could undermine artistic judgment, which they viewed as core to their professional value.
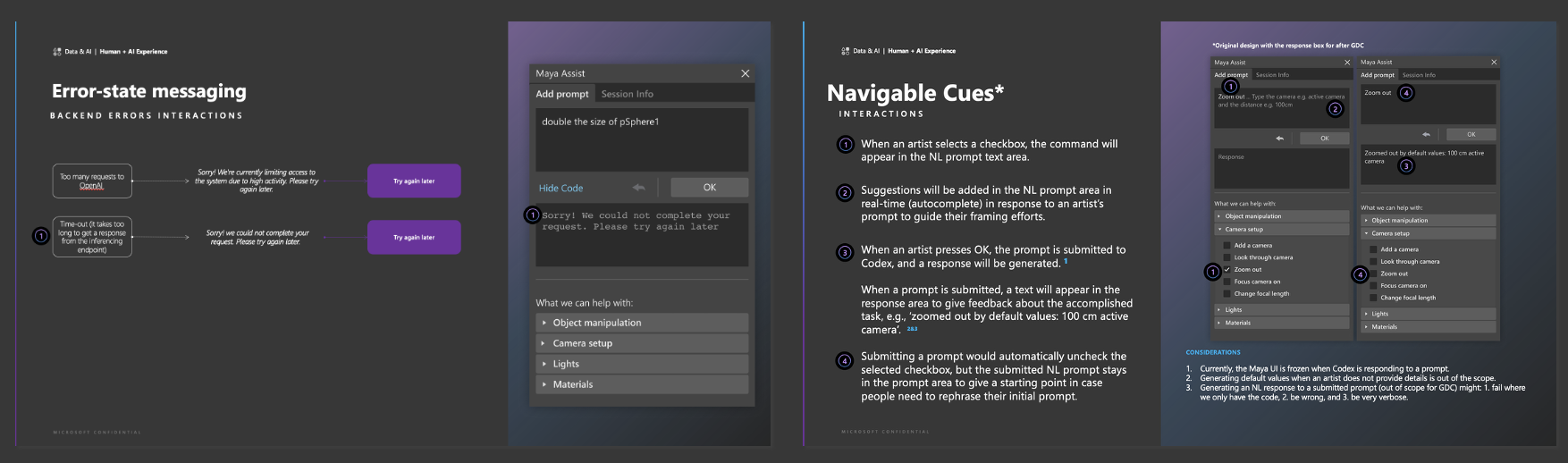
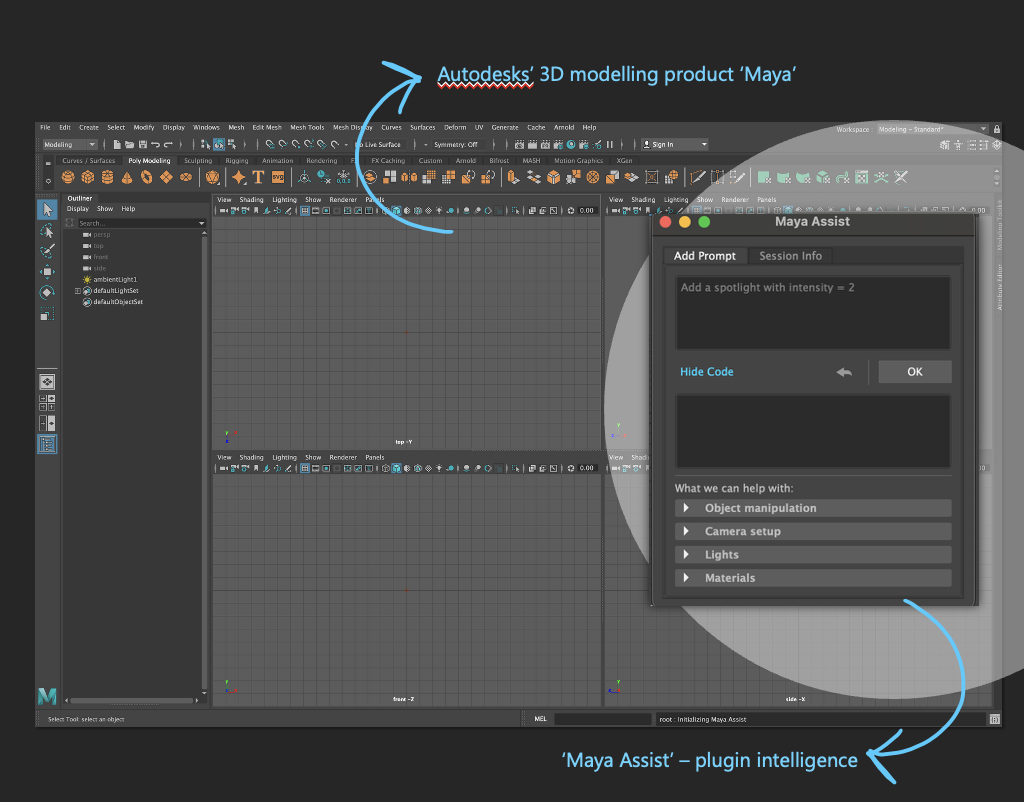
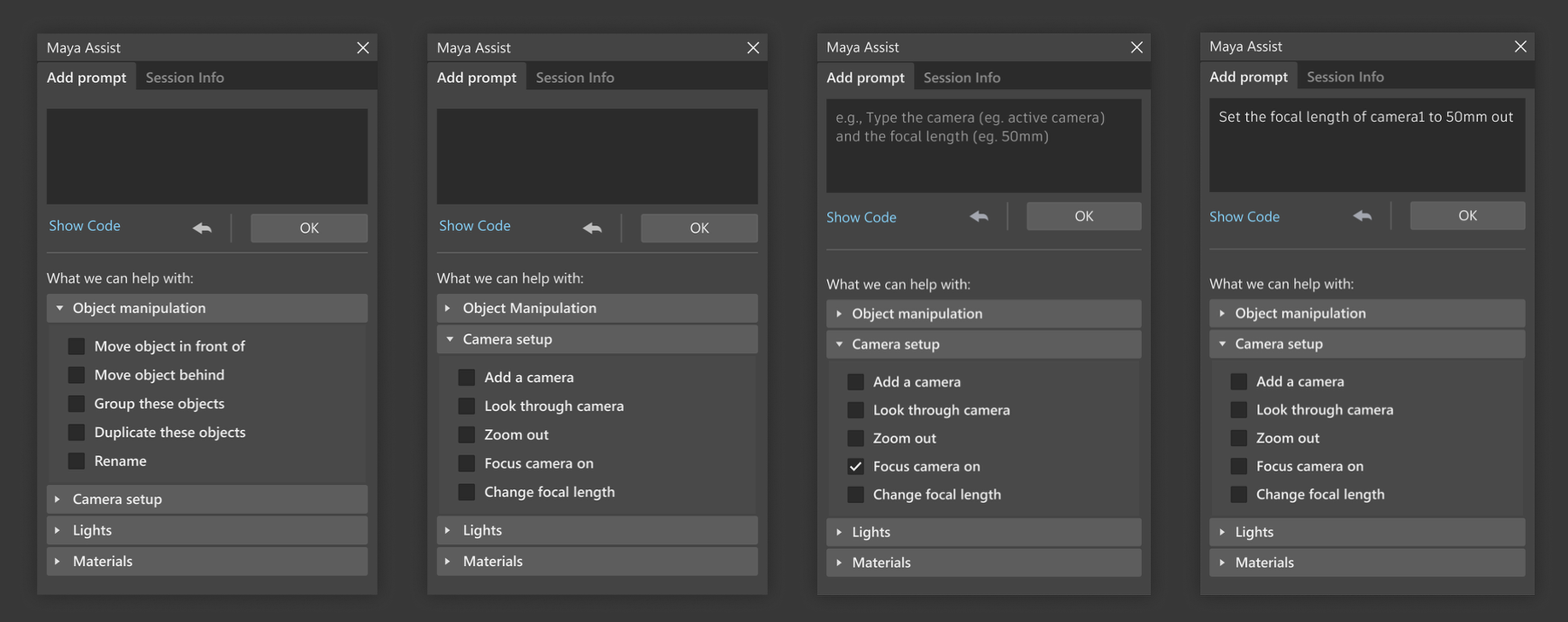
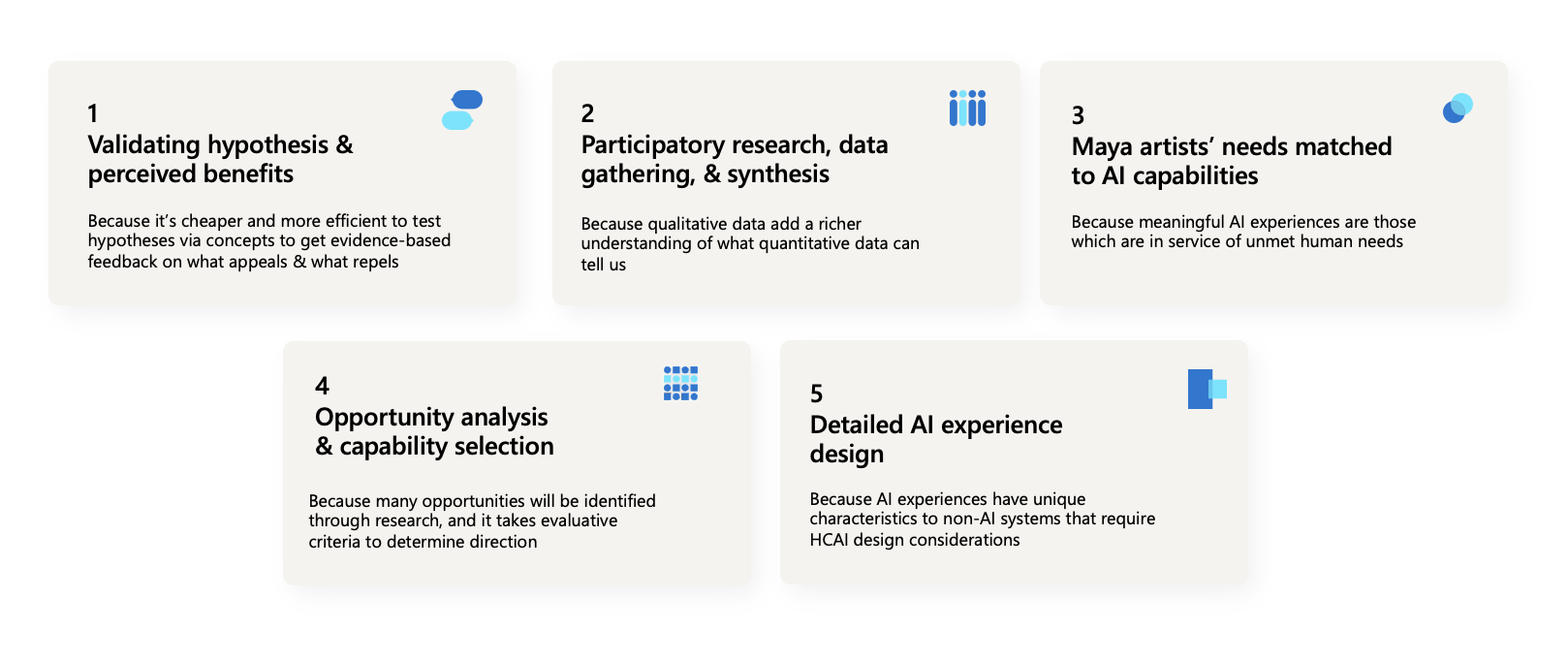
Systems design
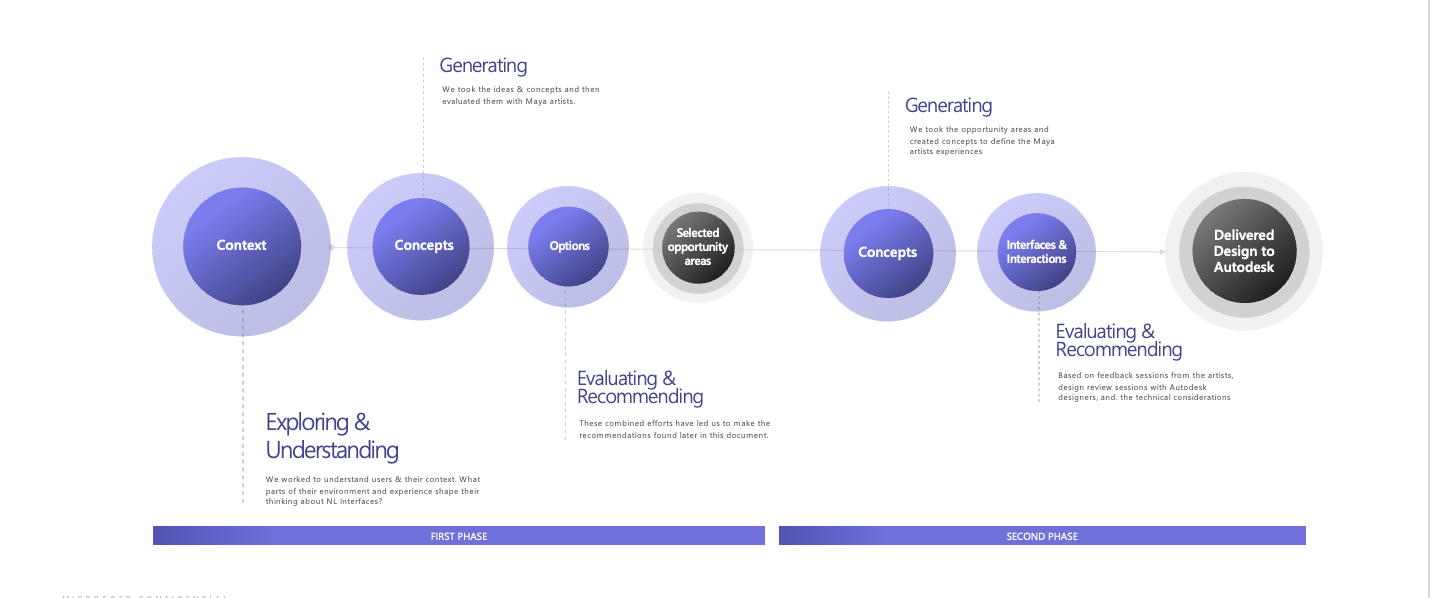
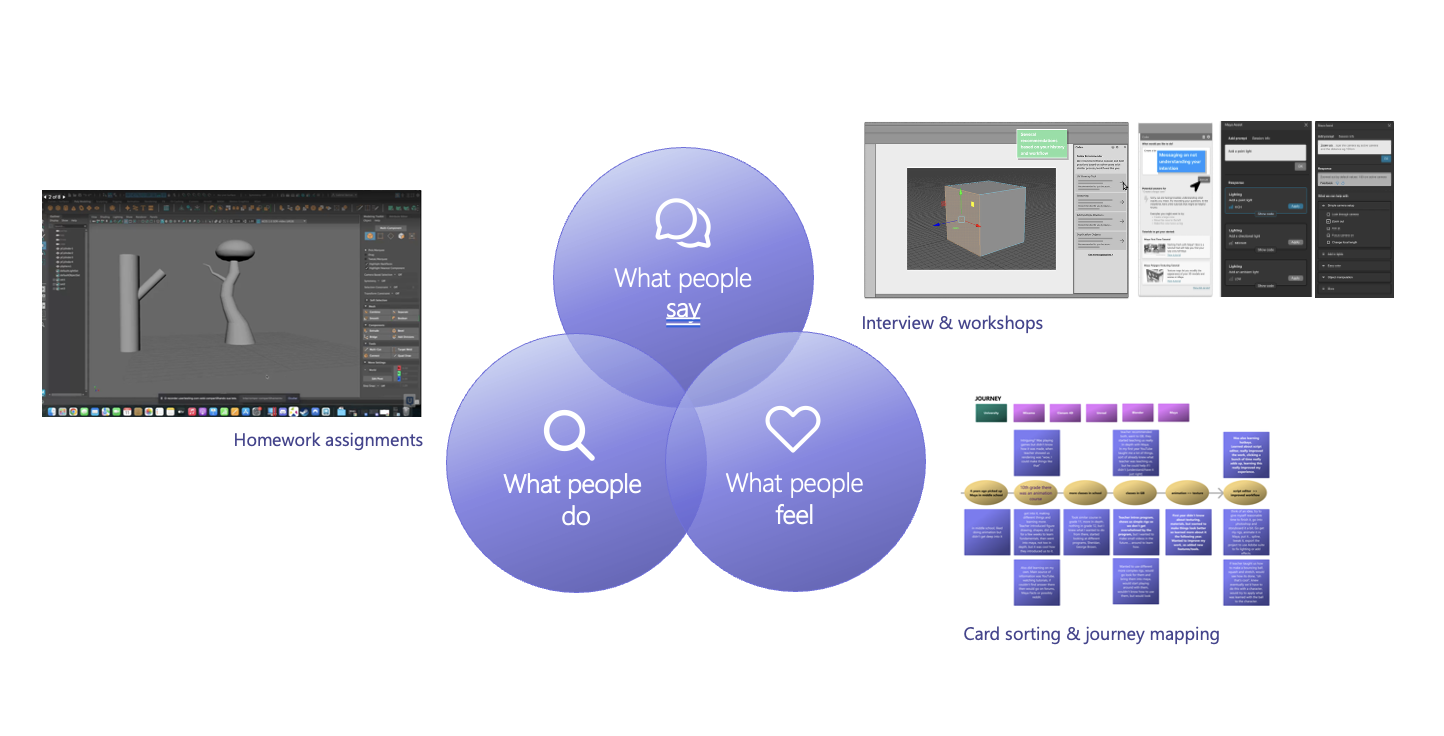
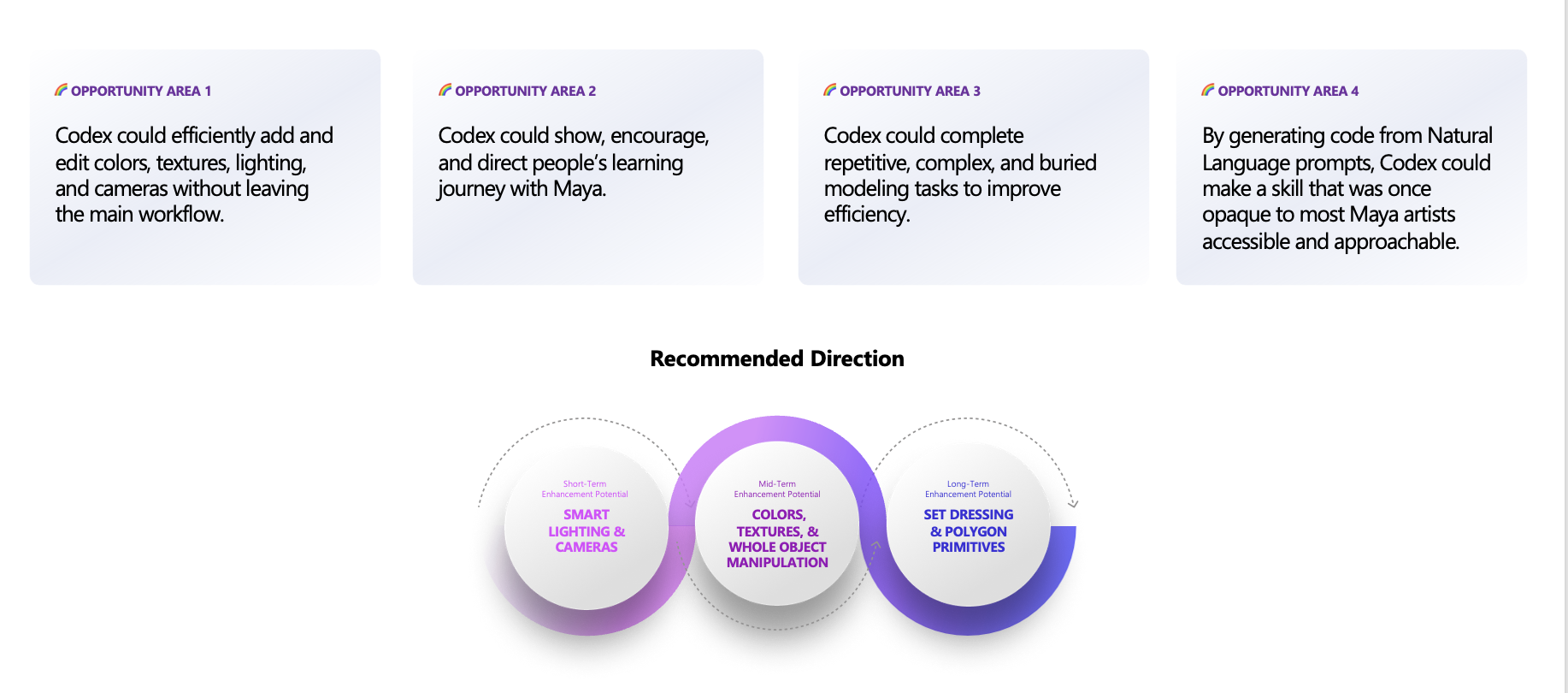
Through interviews, diary studies, and co‑design workshops, the team identified evidence‑based opportunity areas where AI could responsibly assist while preserving artistic control over aesthetic outcomes. The resulting system concept leveraged natural‑language prompts to generate executable code within the primary workflow, enabling artists to complete complex or unfamiliar tasks without leaving the application. RAI considerations, impacting the learning pathways, were incorporated into failure modes, feedback loops, and transparency mechanisms.
Impact
Validation with Maya artists and Autodesk stakeholders informed opportunity selection and feature prioritization, shaping a responsible roadmap for integrating AI assistance into professional creative workflows. The work demonstrated how Human‑AI design can improve learning and efficiency without compromising creative control.

The image was generated with Microsoft Create.
Designing AI‑assisted antibiotic decision support that fits seamlessly into clinical workflows
The problem
Inappropriate antibiotic prescribing often occurs at critical decision points, such as ED‑to‑inpatient admission, where clinicians must rapidly interpret fragmented patient data alongside complex antimicrobial guidelines. While stewardship guidelines are available, they are frequently bypassed due to poor workflow fit, difficult navigation, and the cognitive burden of manually locating diagnosis‑relevant context across the HER.
Systems design
Led the design of an Epic‑aligned RAI stewardship experience by establishing a foundational information architecture composed of three primary data domains: AI Suggestions (e.g., agree/disagree with prior antibiotic choice), Clinical Guidelines (diagnosis and treatment pathways), Patient Data (decision‑relevant clinical context). Through clinician co‑design, structured diagnosis and treatment guidelines were paired with relevant patient data to create an initial information hierarchy supporting context‑aware prescribing decisions and the integration pathways were evaluated across Epic.
Impact
Foster clinical adoption by addressing workflow alignment, epic integration trust, and usability early in the process. Structuring guideline content alongside patient‑specific data enabled context‑aware decisions without overwhelming clinicians, while explainable AI recommendations improved confidence in suggested treatment changes.

The image was generated with Microsoft Create.
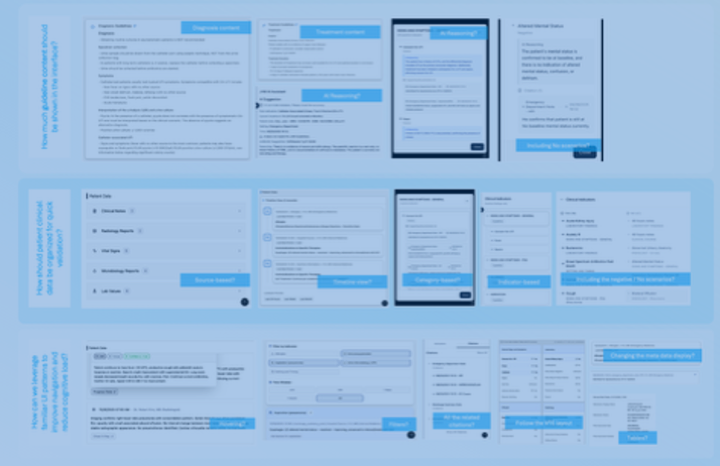
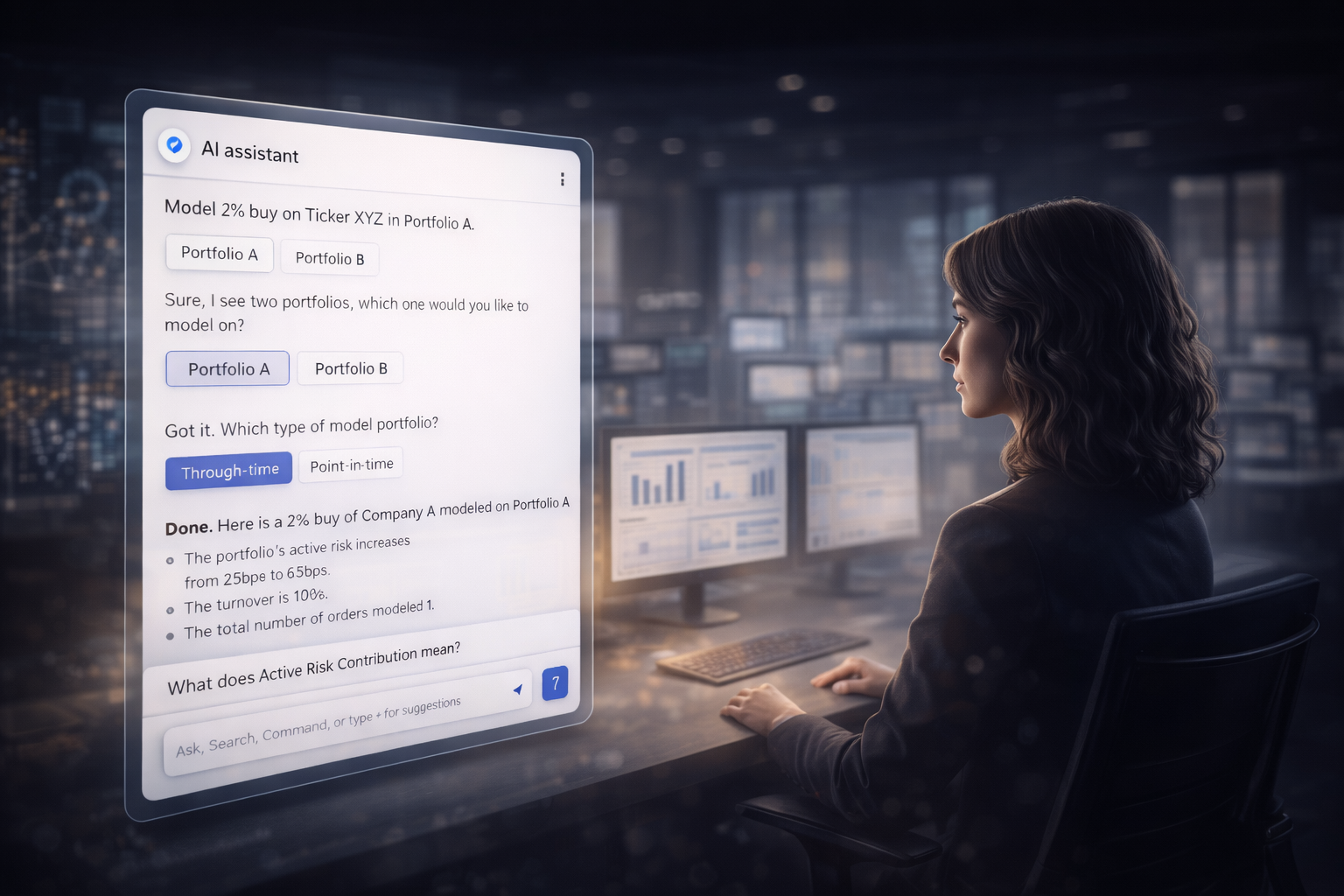
Augmenting investment decision‑making with AI‑driven workflow intelligence
The problem
Investment professionals must make time‑sensitive portfolio decisions while navigating fragmented workflows across a complex suite of financial tools. People often need to switch between multiple applications, interpret large volumes of data, and manually investigate performance disparities — a process that can range from a brief investigation to several hours depending on the number of variables involved. Despite access to extensive documentation and internal support channels, many users lack the time to engage with these resources, creating knowledge gaps and increasing reliance on manual trial‑and‑error processes to complete routine analyses.
Systems design
Through a multidisciplinary discovery and research effort, I led the design‑driven exploration of how an AI assistant could augment portfolio managers’ workflows without replacing human decision‑making. Partnering with product, engineering, and user research teams, we conducted exploratory interviews with portfolio managers and risk analysts to understand mental models, trust boundaries, and opportunities for AI‑assisted support. Insights informed the prioritization of a Minimum Viable Experiment (MVE) focused on enabling natural‑language interaction with platform capabilities, allowing users to query portfolio constraints and generate “what‑if” scenarios without navigating multiple applications. Design choices emphasized transparency and user oversight, ensuring the assistant supported informed decision‑making while leaving execution and regulatory validation with the investment team.
Impact
- The engagement aligned cross‑functional stakeholders around high‑value AI use cases and informed the technical feasibility of integrating a chat‑based assistant into existing workflows.
- Research highlighted time‑saving as the primary expected benefit of an AI assistant and surfaced opportunities to streamline historical data retrieval, automate low‑complexity analytical tasks, and reduce investigation time, enabling investment professionals to focus on higher‑order decision‑making activities.
- The work established an experimentation pathway for AI‑assisted analysis, improving efficiency across portfolio management workflows.
IDEO
Project details are presented at a high level to maintain confidentiality. Additional information is available upon request.
Essential Inc.
Project details are presented at a high level to maintain confidentiality. Additional information is available upon request.